Nov 24, 2025
Bipolar disorder presents as a chronic psychiatric condition marked by recurrent, alternating episodes of depression and mania [13]. Mental health clinicians recognize that traditional symptom checklists miss the full picture of this condition, which affects multiple biological, psychological, and social systems at once.
Years of clinical practice have led me to develop a System Disorder Template that moves beyond basic symptom identification. This template tackles mood fluctuations alongside underlying risk factors—genetics, physiological components, and environmental stressors [13] that trigger manic or depressive episodes. My approach also addresses serious complications ranging from physical exhaustion to potential death [13] when treatment is delayed.
This article presents a structured framework that changes how we assess, document, and treat bipolar disorder. You'll gain a practical, ready-to-use template that covers all critical aspects of care—from neurobiological factors to social context—instead of depending solely on DSM criteria.
This system-based approach prevents common mistakes like misdiagnosis. It provides clearer direction for both medication management and therapeutic interventions.
Why Symptom Checklists Miss the Mark
Traditional symptom checklists fall short when diagnosing bipolar disorder. Clinical experience reveals a significant gap between diagnostic criteria and what patients actually experience.
DSM-5 criteria vs patient reality
The DSM-5 creates diagnostic barriers despite good intentions. The manual now requires both mood change and persistently increased activity or energy levels for diagnosing mania or hypomania [13]. This restrictive "gate criterion" contradicts available evidence and excludes patients who previously qualified for diagnosis [13].
Duration requirements lack scientific support. The four-day minimum for hypomania has no solid foundation. Studies show hypomanic states lasting less than 4 days don't differ from those lasting four or more days [13]. 43.7% of bipolar II patients never experienced a hypomanic episode longer than 2 days [13].
This creates a diagnostic paradox. A patient with a classic hypomanic episode lasting 2-3 days cannot receive a bipolar II diagnosis despite identical symptoms [13]. These constraints mean DSM-IV could formally diagnose under half of patients actually receiving treatment [13].
Patient experiences rarely fit diagnostic boxes. Symptoms fluctuate in intensity and presentation. Mixed states blend depression and hypomanic features, particularly common in bipolar II disorder [1].
Frequent misdiagnoses
Diagnostic limitations have serious consequences. Approximately 40% of bipolar disorder patients receive an initial diagnosis of unipolar depression [1]. This happens because bipolar disorder often starts with a depressive episode [4], and depressive symptoms occur more frequently than elevated mood symptoms [4].
Accurate diagnosis takes over seven years on average [9]. This delay has dangerous consequences. Treating with antidepressants without mood stabilizers can trigger mania [9]. One study found 55% of misdiagnosed bipolar patients developed mania after antidepressant treatment, with 23% becoming rapid cyclers [1].
ADHD presents another diagnostic challenge. The conditions share substantial symptom overlap—1 in 6 bipolar patients also have ADHD, and 1 in 13 ADHD patients also have bipolar disorder [1]. Mania in children often looks like ADHD hyperactivity and impulsivity [2].
Several factors complicate diagnosis:
Patients rarely seek help during hypomanic episodes, viewing them as positive states [4]
Clinicians don't routinely screen for bipolar disorder in depressed patients [9]
Hypomania gets forgotten or isn't recognized as illness [4]
Other conditions mask mania or hypomania [4]
The case for systems-based assessment
Symptom checklists clearly aren't enough. A systems-based clinical framework offers better diagnostic accuracy and treatment planning.
Effective assessment requires multiple domains: neurobiological factors (family history, age of onset), cognitive-emotional patterns, behavioral functioning, and social-environmental context. This approach captures interactions between different systems that create each patient's unique presentation.
Examining symptoms across domains helps distinguish overlapping conditions. Bipolar depression and unipolar depression share symptoms, but research shows key differences: earlier age of onset (24 versus 30 years) [4], more anxiety and substance use disorders, and worse social functioning in bipolar disorder [4].
Systems thinking reveals subtle indicators of bipolarity in seemingly "unipolar" patients: subthreshold manic symptoms, onset before age 25, family history of bipolar disorder, multiple depression recurrences, and poor antidepressant response [4].
This framework captures nuanced presentations that checklists miss, improving both diagnostic accuracy and patient outcomes.
The Core Template: A Multi-System Assessment Framework
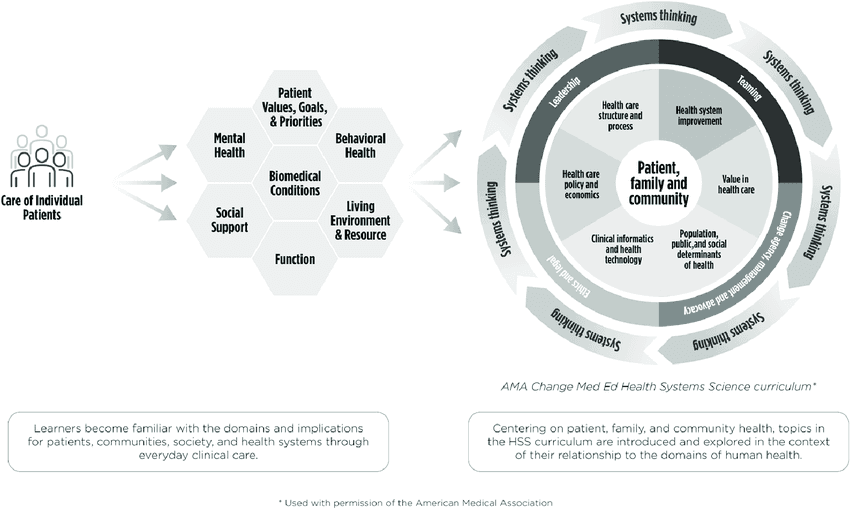
Image Source: www.sap2.org.ar
Complex bipolar cases have shown me that effective assessment requires moving beyond isolated symptoms. Years of refinement have led to a multi-system assessment template that organizes bipolar disorder's complexity into four interconnected domains.
Domain 1: Neurobiological Core – family history, age of onset, psychotic features
The neurobiological domain establishes the foundation of bipolar vulnerability. Twin studies show heritability accounts for 70-80% of bipolar disorder development [2]. First-degree relatives face a 9-10 fold increased risk compared to the general population [9]. This genetic loading creates particular patterns of onset and progression.
Age of onset delivers crucial diagnostic information. Most patients experience their first episode between ages 20-30 [10]. Symptoms frequently begin earlier, though, with the prodromal phase appearing in adolescence. Childhood onset suggests a potentially more severe illness trajectory.
I assess for psychotic features in this domain, which occur in both manic and depressive episodes [1]. Psychosis indicates greater neurobiological disruption and requires different treatment approaches. First-episode psychotic mania predicts more rapid recurrence [2].
Domain 2: Cognitive & Emotional Profile – thought patterns, emotional regulation
Cognitive dysfunction represents a core feature that persists even during mood stability [1]. My assessment targets specific deficits in attention, processing speed, verbal learning, and executive function [11]. These impairments strongly predict functional outcomes.
Affective lability stands out in the emotional sphere—rapid, unpredictable mood intensity changes regardless of circumstances. This has emerged as one of the strongest predictors of bipolar diagnosis [2]. Unlike DSM-5's duration-specific criteria, identifying these autonomous mood shifts provides a more accurate clinical picture.
Comorbidities require special attention here. 50-70% of patients have concurrent psychiatric conditions [4]. Anxiety disorders affect 70-90% of bipolar patients [4], which fundamentally alters presentation and prognosis.
Domain 3: Behavioral & Functional Footprint – work, finances, self-care
Daily functioning impact creates a distinctive behavioral footprint. Approximately half of patients report significant employment difficulties [7]. Unemployment rates run three times higher than the general population [7]. Even during euthymia, executive dysfunction interferes with basic daily tasks [13].
Financial management provides another crucial assessment window. I look particularly at excessive spending patterns during hypomanic or manic states. Self-care routines fluctuate dramatically with mood states—from meticulous attention during hypomania to severe neglect during depression.
Cognitive impairment represents one of the strongest predictors of psychosocial disability [13]. Executive dysfunction correlates most consistently with real-world functional limitations. It affects academic performance [13], vocational outcomes [13], and quality of life [13].
Domain 4: Social & Environmental Context – support systems, stressors
Social environment substantially influences both onset and course. Life events—negative and positive—can trigger mood episodes [1]. Social support significantly impacts relapse rates [1]. I examine relationship quality, as high expressed emotion within families predicts poorer outcomes [1].
Childhood adversity deserves particular attention. Approximately half of people with bipolar disorder report severe childhood abuse history [2]. Early trauma correlates with earlier age of onset and more severe manic symptoms during adolescence [2]. It also increases likelihood of future hypomanic symptoms [2].
Social rhythm disruptions represent another key environmental trigger. Events that disrupt regular sleep, meal, and social interaction patterns can precipitate mood episodes [2]. Goal attainment life events appear particularly potent in triggering manic symptoms compared to general positive events [2].
Systematic assessment across these four domains creates a complete clinical picture. This captures the full complexity of each person's bipolar presentation, ultimately guiding more precise and effective treatment decisions.
Building Treatment Plans with the Template
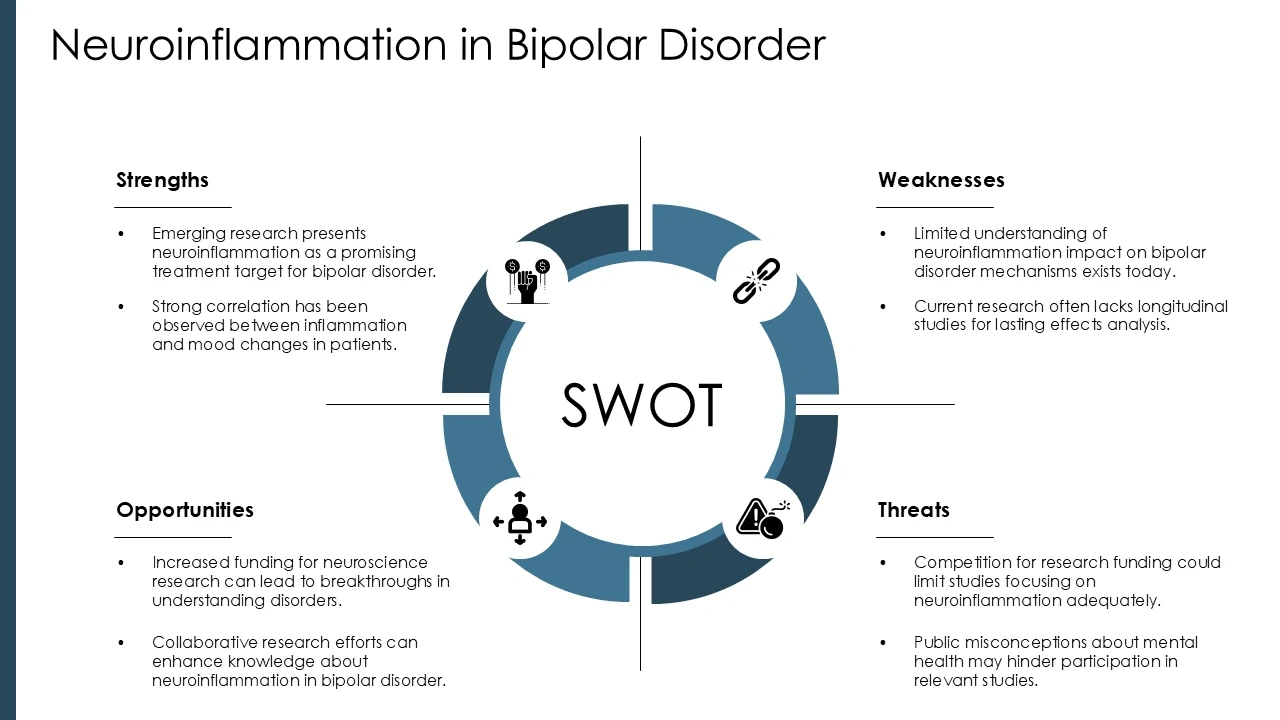
Image Source: SlideTeam
Once the multi-domain assessment is complete, the next step focuses on creating an actionable treatment plan. The system disorder template functions as both diagnostic framework and intervention roadmap, ensuring treatment addresses all affected domains rather than isolated symptoms.
Connecting Domains to DSM-5 Diagnosis Codes
Accurate diagnosis coding establishes the foundation for treatment planning. Our template links assessment findings to specific ICD-10 codes, creating clear documentation that supports clinical decisions and insurance requirements. Bipolar I disorder codes range from F31.0 (current episode hypomanic) to F31.64 (current episode mixed with psychotic features) [14]. Bipolar II disorder uses a single code—F31.81—though clinicians should document current episode characteristics [14].
When documenting, I pair codes with specific domain findings. A patient presenting with severe manic symptoms and family history of bipolar disorder might receive code F31.13 (bipolar I, current episode manic, severe) with additional notes about neurobiological risk factors. This structured approach ensures clear communication with other providers and establishes justification for treatment decisions.
Creating Problem Statements and Measurable Goals
Effective treatment plans convert assessment findings into concrete problem statements and SMART goals (Specific, Measurable, Achievable, Relevant, Time-bound) for each affected domain [15]. Research shows two distinct patterns of patient preferences—some prioritize symptom management while others focus on social functioning improvement [16].
Each domain receives targeted goals:
Neurobiological Domain: "Achieve mood stability within four weeks through medication adherence" or "Reduce frequency of manic episodes by 50% over six months" [17]
Cognitive-Emotional Domain: "Decrease intensity of emotional reactivity as measured by daily mood ratings" or "Improve executive functioning to complete daily tasks independently"
Behavioral Domain: "Restore consistent sleep schedule within three weeks" or "Return to baseline occupational functioning within three months" [18]
Social Domain: "Rebuild relationship with significant other through weekly structured communication practice" or "Develop three new stress-management strategies within supportive social contexts" [16]
Treatment plans should acknowledge different patient priorities. While symptom reduction remains important, research indicates many patients place greater importance on reducing impulsivity (score: 9.73) or regaining the ability to feel pleasure (score: 9.54) than on reducing medication side effects (score: ≤4.51) [16].
Selecting Interventions Across Multiple Modalities
A complete bipolar treatment plan integrates interventions across multiple modalities. Medication typically serves as the cornerstone, with mood stabilizers (lithium, valproate, lamotrigine), antipsychotics, and occasionally antidepressants (with caution) addressing neurobiological symptoms [19]. Medication choice must be personalized—studies show up to 25% of patients relapse within the first year even with pharmacotherapy, while relapse rates exceed 70% within five years regardless of treatment approach [20].
Psychotherapy provides essential support, with research indicating faster recovery and better medication adherence when therapy is included [3]. Evidence supports several approaches:
• Cognitive-behavioral therapy for managing thoughts and behaviors • Interpersonal and social rhythm therapy for stabilizing daily routines
• Family-focused therapy for improving home environment and communication [3]
Social and environmental interventions complete the plan, including psychoeducation for patients and families, lifestyle management strategies, and structured support systems [21]. A complete approach coordinates across healthcare providers, ensuring physical health metrics are integrated with psychiatric care [3].
This template application moves clinicians beyond symptom suppression toward addressing the full complexity of bipolar disorder across all affected life domains.
Critical Risks in Bipolar Disorder Management
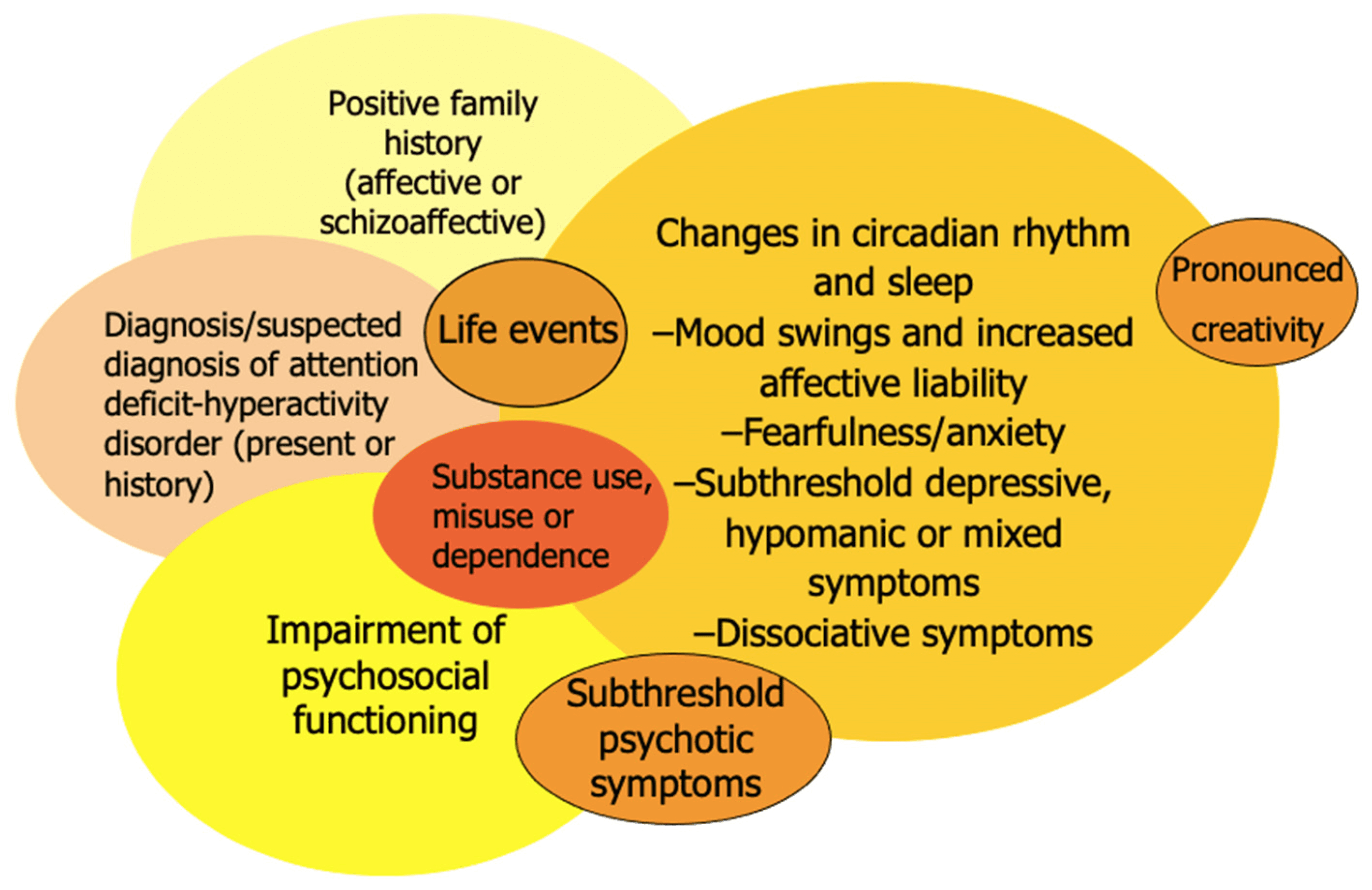
Image Source: MDPI
Bipolar disorder management presents specific risks that can significantly impact treatment outcomes. My clinical practice has revealed three particularly concerning pitfalls that demand careful attention.
Risk of misdiagnosing bipolar depression as unipolar
Misdiagnosis stands as one of the most serious challenges in bipolar care. Nearly 70% of bipolar patients receive incorrect initial diagnoses, with over one-third still unidentified a decade later [22]. This diagnostic delay creates problems that cascade through the entire treatment process.
Misdiagnosing bipolar depression as unipolar depression carries consequences beyond delayed treatment. Inappropriate antidepressant monotherapy can trigger manic episodes in bipolar patients [23]. Studies confirm that antidepressants may induce manic or hypomanic episodes, potentially altering the illness course [23].
Specific clinical features should raise suspicion for bipolar disorder in patients presenting with depression:
Earlier age of onset
Family history of bipolar disorder
Multiple recurrent depressive episodes
Presence of psychotic symptoms [24]
Comorbidities often mask or confuse affective symptoms, increasing misdiagnosis rates [24].
Overlooking medical comorbidities like thyroid or metabolic issues
Physical health monitoring often gets neglected in bipolar management. Approximately 90% of bipolar patients have at least one medical comorbidity [25], with endocrine/metabolic and vascular diseases particularly common [25].
Thyroid dysfunction requires special attention in bipolar patients, with prevalence ranging from 10-30% [26]. This relationship works both ways—thyroid issues may contribute to mood instability, while bipolar treatments (especially lithium) can cause hypothyroidism [5].
Bipolar patients face elevated risks for several conditions:
Migraine headaches (23.7%) [6]
Asthma (19.2%) [6]
Elevated lipids (19.2%) [6]
Hypertension (15%) [6]
These medical comorbidities worsen illness course, delay rehabilitation, prolong hospitalization, increase recurrence risk, and elevate suicide rates [27]. Individuals with serious mental illness now die approximately 25 years earlier than the general population, with up to 60% of these premature deaths resulting from general medical conditions [6].
Therapeutic rupture from invalidating manic experiences
The therapeutic alliance between clinician and patient predicts treatment outcomes, yet alliance ruptures occur frequently in bipolar disorder treatment [28]. These ruptures range from subtle strains to complete trust breakdowns [28].
A primary rupture source involves invalidating patients' lived experiences of mania. For many individuals with bipolar disorder, mania represented relief from depression before diagnosis—a period of feeling good, productive, and accomplished [12]. When clinicians dismiss these experiences or attribute all patient behaviors to their illness, essential trust erodes [12].
Patients consistently report feeling invalidated by statements like "That's just the bipolar talking" or "Have you taken your meds?" [12]. This dismissal of legitimate feelings and experiences leads to shame, isolation, and treatment disengagement [12].
Maintaining therapeutic alliance requires acknowledging the complexity of bipolar experiences. Effective clinical practice recognizes that medication helps manage extremes rather than curing everything, validates emotional experiences while addressing harmful behaviors, and understands that mania has both positive and negative aspects for patients [12].
Clinical Tools and Documentation Strategies

Image Source: Best Nursing Essay Writing Service for Studying Nurses
Effective bipolar disorder management relies on the right clinical tools and solid documentation practices. Standardized screening instruments help ensure consistency in diagnosis and ongoing care while reducing the burden on busy practitioners.
Using MDQ and HCL-32 for hypomania screening
Routine screening for bipolar symptoms in depressed patients cuts misdiagnosis rates significantly. Two screening tools stand out for their practical value: the Mood Disorder Questionnaire (MDQ) and 32-item Hypomania Checklist (HCL-32).
The MDQ uses 13 simple yes/no questions that evaluate manic symptoms based on DSM criteria [29]. A positive screen requires seven or more "yes" responses, plus symptoms that cause moderate functional problems. The HCL-32 takes a different approach with 32 possible hypomanic symptoms, also rated yes/no, with scores calculated by adding all "yes" responses [30].
Both tools show reliable results:
HCL-32: sensitivity of 82% and specificity of 57% [31]
MDQ: sensitivity of 80% and specificity of 70% [31]
The MDQ works better in busy primary care settings [32], while the HCL-32 may catch more bipolar II cases [33].
SOAP note example using the system disorder template
The system disorder template transforms standard SOAP notes into complete clinical pictures. I organize my assessment section around the four domains—neurobiological, cognitive-emotional, behavioral-functional, and social-environmental. Each domain gets clear documentation that connects what we observe to the underlying systems involved.
This approach saves time during documentation while ensuring nothing important gets missed. The template structure guides your thinking and creates consistent, thorough records that support treatment decisions and insurance requirements.
Integrating physical health metrics into psychiatric notes
Physical health data belongs in every psychiatric note. I routinely document:
Blood pressure, heart rate, respiratory rate
Temperature and weight changes
BMI calculations [8]
I also include screening scores like PHQ-9 for depression severity, GAD-7 for anxiety, and YMRS for mania intensity [8]. This integration recognizes how closely physical and mental health connect, creating a complete approach to bipolar care that prevents overlooking critical medical issues.
Educating Clients and Families with the Template
Patient and family education stands as a critical element of bipolar management. Psychoeducation interventions, especially those teaching patients to recognize early warning signs (EWS), show significant benefits, including increased time to recurrence and reduced hospitalization rates [34].
Visualizing the system template for psychoeducation
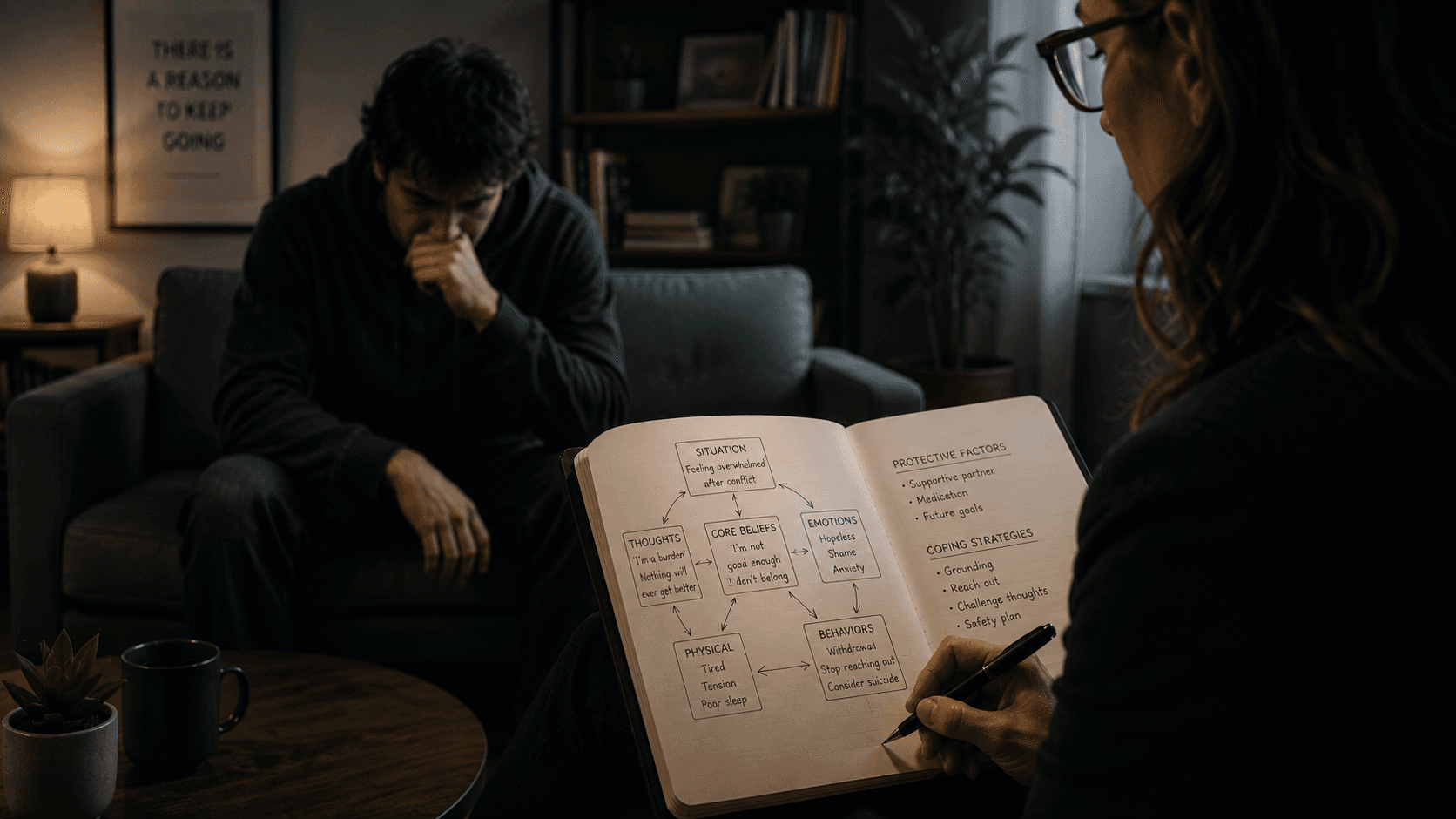
The multi-domain template becomes more effective when converted into visual tools that enhance patient understanding. I create simplified domain maps that show connections between biological vulnerabilities, thought patterns, behavioral changes, and environmental triggers. This visualization helps families see bipolar disorder as a system rather than isolated symptoms.
The Life Goals app provides 5-10 minute modules covering self-management activities and symptom coping strategies that users complete at their own pace [35]. Visual tools make complex relationships clear and accessible.
Collaborative goal setting using domain-based language
Collaborative care models offer an evidence-based approach to structuring bipolar treatment [36]. When setting goals, I use domain-specific language that connects with patients' lived experience. Together, we identify specific self-management goals for each domain, focusing on aspects patients can control.
This approach builds empowerment while recognizing the need for ongoing management. Life Goals Collaborative Care (LGCC) uses this methodology by helping patients align symptom coping strategies with personal goals [35]. Domain-based language creates clarity about what patients can influence directly.
Teaching early warning signs across domains
Early warning sign recognition forms the foundation of relapse prevention. I teach patients that EWS identification takes time, effort, and persistence [37]. We develop mindfulness skills to maintain awareness of thoughts, feelings, and behaviors [37].
We track these signs across all domains:
Biological (sleep changes)
Cognitive (racing thoughts)
Behavioral (increased activity)
Social (relationship conflicts)
Patients who effectively manage prodromal symptoms show improved social and occupational function [34]. This domain-based approach helps patients recognize patterns before episodes escalate.
Conclusion
Years of clinical work with bipolar patients have shown me that this System Disorder Template changes how we approach care. The framework moves beyond symptom-focused interventions toward complete assessment across multiple domains. Bipolar disorder affects not just mood, but entire biological, cognitive, behavioral, and social systems at once.
DSM-5 criteria alone miss crucial aspects of patient experience. Misdiagnosis rates remain alarmingly high, particularly when bipolar depression gets confused with unipolar depression. The multi-domain assessment outlined here reduces these diagnostic errors while providing clear treatment direction.
Each domain serves a specific purpose. The neurobiological domain captures genetic vulnerabilities and age of onset, establishing the foundation for medication strategies. The cognitive-emotional profile maps thought patterns and emotional regulation capacities, guiding therapeutic interventions. The behavioral and functional footprint reveals real-world impacts on work, finances, and self-care, helping clinicians target practical life skills. The social and environmental context illuminates support systems and stressors essential for sustainable recovery.
Clinicians who adopt this systems approach report greater confidence in their assessment process. Patients experience validation as their complex experiences receive proper acknowledgment rather than reduction to symptom checklists. Implementing this framework requires initial time investment, but pays dividends through more accurate diagnosis, targeted interventions, and reduced recurrence rates.
Documentation using this template creates a thorough clinical picture that supports both treatment planning and insurance requirements. Structured notes facilitate better communication between providers and ensure continuity of care across treatment settings.
The System Disorder Template serves as both clinical guide and educational tool. Sharing domain-specific visuals with patients and families enhances understanding of this complex condition. Collaborative goal setting across domains empowers patients as active participants rather than passive recipients of care.
Ready to enhance your bipolar disorder assessments and improve patient outcomes? The multi-domain approach outlined in this template provides the structured framework you need to move beyond symptom checklists toward truly effective care.
Mental health professionals deserve tools that match the complexity of the conditions they treat. This system-based approach helps you provide the thorough, compassionate care your bipolar patients need while ensuring nothing critical gets overlooked in the assessment and treatment process.
Experience how modern AI technology can support your clinical documentation and enhance your therapeutic insights. Yung Sidekick automatically generates comprehensive progress notes and therapy reports that align with systematic assessment frameworks like this template. Our AI captures session details while you stay fully present with your clients, ensuring thorough documentation that supports better patient outcomes.
Key Takeaways
Traditional symptom checklists fail to capture bipolar disorder's complexity, leading to 40% misdiagnosis rates and seven-year diagnostic delays that can worsen patient outcomes.
• Move beyond DSM-5 limitations: Use a four-domain assessment framework covering neurobiological, cognitive-emotional, behavioral-functional, and social-environmental factors instead of relying solely on symptom checklists.
• Screen systematically for hypomania: Implement tools like MDQ and HCL-32 to identify missed bipolar cases, especially in patients presenting with depression who may have unrecognized hypomanic episodes.
• Address medical comorbidities: Monitor thyroid function and metabolic health, as 90% of bipolar patients have medical comorbidities that can worsen illness course and increase mortality risk.
• Validate patient experiences: Avoid therapeutic ruptures by acknowledging both positive and negative aspects of manic episodes rather than dismissing all behaviors as "just the bipolar talking."
• Integrate comprehensive documentation: Structure SOAP notes around the four-domain template and include physical health metrics to create holistic treatment plans that prevent overlooking critical factors.
This systems-based approach transforms bipolar care from symptom management to comprehensive treatment addressing the full complexity of how this condition impacts multiple life domains simultaneously.
FAQs
What are the key domains to assess when evaluating bipolar disorder?
The article outlines four key domains for assessing bipolar disorder: the neurobiological core (including family history and age of onset), cognitive and emotional profile, behavioral and functional footprint, and social and environmental context. This multi-system approach provides a more comprehensive understanding of the disorder beyond traditional symptom checklists.
How can misdiagnosis of bipolar disorder be reduced?
Misdiagnosis can be reduced by using screening tools like the Mood Disorder Questionnaire (MDQ) and Hypomania Checklist (HCL-32), especially for patients presenting with depression. Additionally, clinicians should be aware of features that may indicate bipolarity, such as earlier age of onset, family history, and multiple recurrent depressive episodes.
Why is it important to monitor physical health in bipolar patients?
Physical health monitoring is crucial because approximately 90% of bipolar patients have at least one medical comorbidity. Conditions like thyroid dysfunction, metabolic issues, and cardiovascular diseases are common and can significantly impact the course of bipolar disorder and overall patient health.
How can clinicians maintain a strong therapeutic alliance with bipolar patients?
Clinicians can maintain a strong alliance by validating patients' experiences of mania, acknowledging both positive and negative aspects, and avoiding dismissive statements. It's important to recognize the complexity of bipolar experiences and not attribute all patient behaviors solely to their illness.
What role does psychoeducation play in bipolar disorder management?
Psychoeducation is critical in bipolar management. It involves teaching patients and families about the disorder using visual tools, collaborative goal setting, and early warning sign recognition across all domains. This approach empowers patients, improves self-management, and can lead to better long-term outcomes.
References
[1] - https://www.studocu.com/en-us/document/raritan-valley-community-college/fundamentals-of-nursing/bipolar-ati-system-disorder/13889039
[2] - https://edubirdie.com/docs/minnesota-state-university-moorhead/psy-465-clinical-psychology/116968-bipolar-system-disorder-ati-template
[3] - https://pmc.ncbi.nlm.nih.gov/articles/PMC4230689/
[4] - https://journals.sagepub.com/doi/10.1177/0004867418808382
[5] - https://psychiatryonline.org/doi/10.1176/appi.pn.2023.03.3.22
[6] - https://pmc.ncbi.nlm.nih.gov/articles/PMC2945875/
[7] - https://www.uptodate.com/contents/bipolar-disorder-in-adults-assessment-and-diagnosis
[8] - https://pmc.ncbi.nlm.nih.gov/articles/PMC2847794/
[9] - https://goodhealthpsych.com/blog/adhd-vs-bipolar-key-differences/
[10] - https://childmind.org/article/bipolar-disorder-difficult-to-diagnose-in-adolescents/
[11] - https://www.aafp.org/pubs/afp/issues/2021/0215/p227.html
[12] - https://pmc.ncbi.nlm.nih.gov/articles/PMC5755726/
[13] - https://www.frontiersin.org/journals/psychiatry/articles/10.3389/fpsyt.2023.1253088/full
[14] - https://pmc.ncbi.nlm.nih.gov/articles/PMC7167807/
[15] - https://link.springer.com/article/10.1007/s44192-022-00010-5
[16] - https://psychiatryonline.org/doi/10.1176/appi.focus.20230012
[17] - https://www.sciencedirect.com/science/article/abs/pii/S0022395622006987
[18] - https://www.ncbi.nlm.nih.gov/books/NBK558998/
[19] - https://pmc.ncbi.nlm.nih.gov/articles/PMC10726715/
[20] - https://pmc.ncbi.nlm.nih.gov/articles/PMC3180778/
[21] - https://psychcentral.com/bipolar/dsm-5-diagnostic-codes-for-bipolar-disorder
[22] - https://www.blueprint.ai/blog/bipolar-treatment-plan-example-and-template-for-therapists
[23] - https://pmc.ncbi.nlm.nih.gov/articles/PMC10578617/
[24] - https://www.mentalyc.com/blog/how-to-write-a-treatment-plan-for-bipolar-disorder
[25] - https://www.upheal.io/blog/treatment-plan-for-bipolar-disorder
[26] - https://www.mayoclinic.org/diseases-conditions/bipolar-disorder/diagnosis-treatment/drc-20355961
[27] - https://www.helpguide.org/mental-health/bipolar-disorder/bipolar-disorder-treatment
[28] - https://www.mind.org.uk/information-support/types-of-mental-health-problems/bipolar-disorder/treatment-for-bipolar/
[29] - https://www.usmedicine.com/related/bipolar-disorder-often-misdiagnosed-as-major-depression-leading-to-improper-treatment/
[30] - https://www.thelancet.com/journals/eclinm/article/PIIS2589-5370(25)00345-1/fulltext
[31] - https://pmc.ncbi.nlm.nih.gov/articles/PMC5936046/
[32] - https://www.sciencedirect.com/science/article/pii/S2666915320300019
[33] - https://pmc.ncbi.nlm.nih.gov/articles/PMC11468925/
[34] - https://www.healthcentral.com/condition/bipolar-disorder/thyroid-and-bipolar
[35] - https://pmc.ncbi.nlm.nih.gov/articles/PMC4248234/
[36] - https://bmcpsychiatry.biomedcentral.com/articles/10.1186/s12888-022-03819-0
[37] - https://www.psychologytoday.com/us/blog/straight-talk/201801/therapeutic-alliance-ruptures
[38] - https://www.nami.org/Personal-Stories/How-Invalidating-My-Bipolar-Disorder-Invalidates-M
[39] - https://www.camh.ca/en/professionals/treating-conditions-and-disorders/bipolar-disorder/bipolar-disorder-screening-and-assessment
[40] - https://bmcpsychiatry.biomedcentral.com/articles/10.1186/s12888-023-04529-x
[41] - https://pubmed.ncbi.nlm.nih.gov/30684793/
[42] - https://pubmed.ncbi.nlm.nih.gov/24236281/
[43] - https://www.soapnoteai.com/soap-note-guides-and-example/psychiatry/examples/
[44] - https://pmc.ncbi.nlm.nih.gov/articles/PMC6544804/
[45] - https://formative.jmir.org/2021/12/e32450/
[46] - https://pubmed.ncbi.nlm.nih.gov/38754598/
[47] - https://ibpf.org/spotting-icebergs-from-miles-away-how-to-use-early-warning-signs-in-bipolar-disorder-relapse-prevention/
If you’re ready to spend less time on documentation and more on therapy, get started with a free trial today
Not medical advice. For informational use only.
Outline
More articles