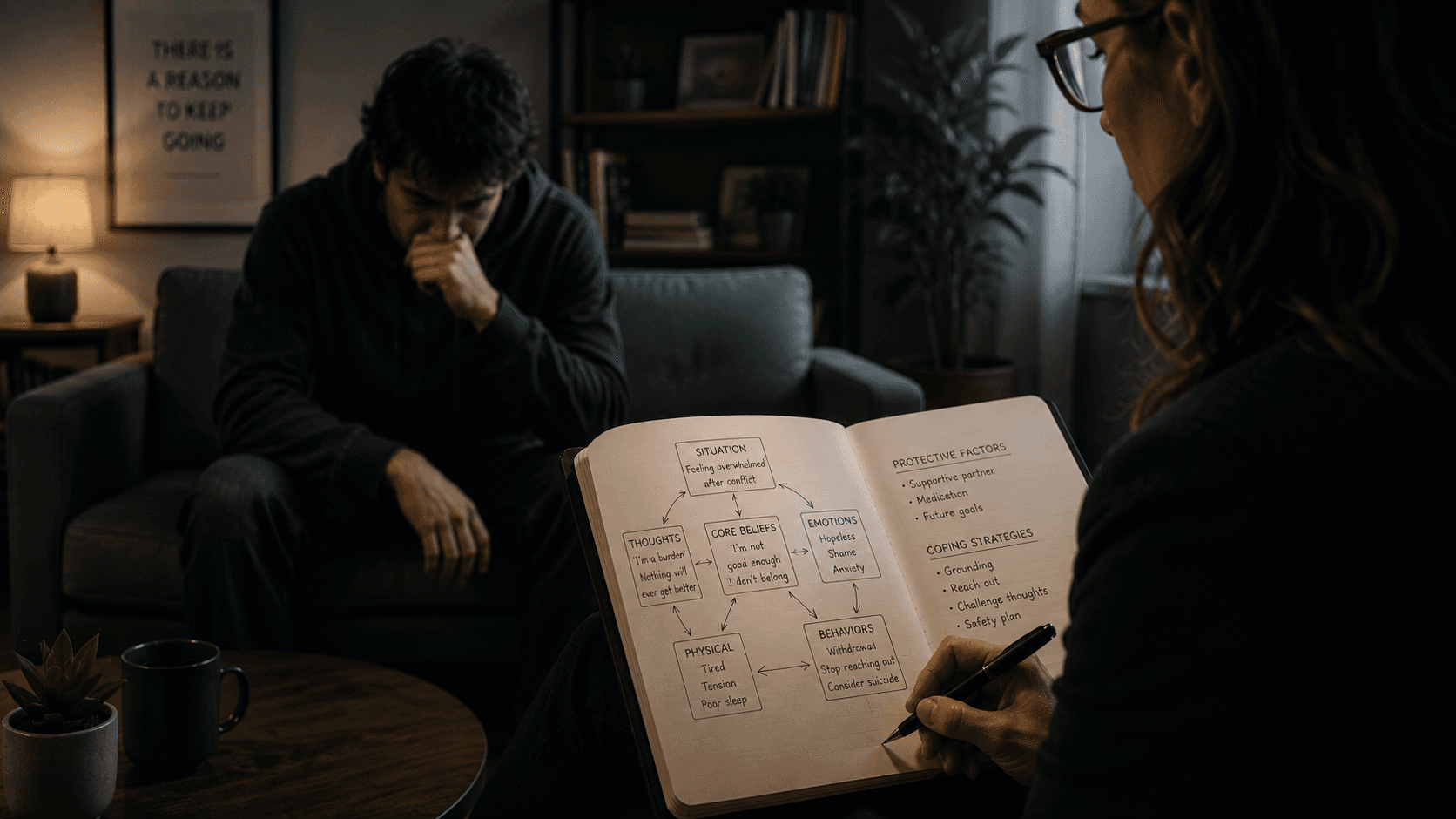
The First Step After Assessment: 3-Session Protocol for Transforming Diagnosis into Therapeutic Momentum

Nov 26, 2025
Did you know that many therapists report spending twice as long on paperwork for client intake compared to regular therapy sessions?
After completing a thorough assessment, you might feel the pressure to immediately dive into therapeutic techniques. However, rushing into interventions without establishing a solid foundation often leads to misalignment, poor client engagement, and even early dropout. Instead of yielding to this "premature action" trap, the first steps in a client's program after the assessment should be carefully structured to transform clinical insights into collaborative momentum.
The critical post-assessment phase deserves more attention than it typically receives. In fact, experienced clinicians increasingly recognize that a well-designed treatment plan is just as important as the interventions themselves. By developing a deliberate approach to those initial sessions, you can significantly reduce the likelihood of relapse or the need for more intensive services later.
This article outlines a practical 3-session therapy framework designed specifically to bridge the gap between assessment and treatment. This protocol will help you translate your clinical case formulation into a shared understanding with your client, establish clear starting points and goals, and create a therapeutic contract that transforms your diagnosis into a collaborative journey toward healing.
Session 1: Build a Shared Case Formulation
Building a shared understanding with your client marks the essential first step in your treatment plan after assessment. Research shows that over 90% of survey respondents preferred healthcare providers who communicated without medical jargon. This striking statistic underscores why your first session should prioritize creating a collaborative case formulation that resonates with your client's experience.
Translate diagnosis into a client-friendly narrative
Case conceptualization (also called case formulation) goes far beyond a simple diagnosis. It weaves together a comprehensive understanding of your client, with the diagnosis representing just one piece of a larger puzzle [2]. This broader framework allows you both to see patterns more clearly and develop a more effective treatment approach.
Begin this session by crafting a narrative that makes sense of the client's experiences. Unlike the assessment phase, where you gathered information, this session focuses on creating meaning together. A well-formulated case conceptualization integrates:
The client's presenting problems and symptoms
Relevant background information and context
The client's strengths and resources
Hypotheses about underlying mechanisms driving the problems
Initial treatment goals [2]
Remember that your role in this process is not to present yourself as the expert who will "fix" the client. Rather, consider yourself a collaborator who brings clinical expertise while acknowledging the client as the authority on their own experiences. As you share your understanding, present it tentatively – as a hypothesis to be refined together.
For example, rather than stating definitively, "You have generalized anxiety disorder," try something like: "Based on what you've shared, it seems your body's alarm system is going off frequently, even in situations that might not warrant such intense reactions. Does that sound accurate to you?"
This collaborative approach serves several purposes. First, it encourages active client participation from the beginning. Second, it demonstrates that you value their input. Finally, it ensures the case formulation actually fits their lived experience, increasing the likelihood they'll engage with treatment.
Use metaphors to explain symptoms and patterns
After developing your initial understanding, the next step involves translating clinical concepts into language that resonates emotionally with your client. Metaphors provide an exceptionally powerful tool for this purpose.
Research indicates that metaphors facilitate therapeutic dialogs and open channels of communication that lead to healing [3]. Furthermore, when metaphors are used to explain complex concepts like pain biology, study participants showed significantly better understanding (73%) compared to those given standard educational materials (43%) [3].
Metaphors work effectively because they connect abstract psychological concepts to concrete, familiar experiences. Additionally, studies have found that real (literal) and symbolic (metaphorical) versions of a concept are processed in the same brain regions, making metaphors particularly powerful for communicating complex ideas [3].
Consider these examples for common presenting problems:
For anxiety: "Your mind's alarm system is like a smoke detector that's become too sensitive – going off at the slightest hint of smoke, even when there's no actual fire."
For depression: "It's as if you're walking through deep mud – each step requires tremendous effort, and the journey feels endless."
For relationship conflicts: "You and your partner have developed a pattern like a dance – one steps forward, the other steps back, each reacting to the other's movements in predictable ways."
Though you can suggest metaphors, the most effective ones often come from clients themselves. Patient-generated metaphors create a "safe bridge" through which they can express emotions that are otherwise difficult to articulate [3]. Pay close attention to the descriptive language your client uses naturally, then build upon those expressions to develop metaphors that truly resonate.
For instance, if a client describes their pain as "burning," you might explore whether they also feel they're "burning with rage" about situations in their life where they've felt wronged or unappreciated [3]. This connection can lead to meaningful insights about how emotional experiences manifest physically.
Different metaphors work better for different therapeutic goals. Research shows that metaphors about struggles can be positive when they reinforce client agency and control over their situation [4]. Similarly, journey metaphors can be positive if the client feels they have direction and control, but negative if they feel they lack agency [4].
Additionally, the metaphors you choose should align with your therapeutic approach. Ultimately, regardless of which metaphors you use, the goal remains the same: to help clients understand their experiences in ways that normalize their reactions while creating hope for change.
Check for understanding and agreement
Once you've presented your case formulation using accessible language and meaningful metaphors, the next crucial step involves verifying that your client genuinely understands and agrees with this shared narrative. Fundamentally, this process should be viewed as collaborative rather than prescriptive.
A key principle of formulation in clinical psychology is that it should be understood in terms of "usefulness" rather than absolute "truth" [5]. In other words, a good formulation isn't necessarily a perfect scientific explanation but rather a "plausible account" that helps the client make sense of their experience and points toward productive change.
To ensure genuine understanding and agreement:
Invite the client to summarize the formulation in their own words
Ask specific questions about parts that might be unclear
Notice non-verbal cues that might indicate confusion or disagreement
Encourage the client to modify or add to the formulation
Throughout this process, remain curious and investigative rather than defensive about your initial hypothesis. Be genuinely open to revising your understanding based on new information or the client's feedback. As one set of clinical guidelines states, formulation should be "revised as necessary in light of new information" [5].
For example, you might ask: "How does this explanation fit with your own understanding of what you've been experiencing?" or "Is there anything important I might be missing or misunderstanding about your situation?"
This verification step serves several vital purposes beyond simply checking comprehension. First, it demonstrates respect for the client's perspective and agency. Second, it strengthens the therapeutic alliance by establishing therapy as a collaborative endeavor. Third, it increases the likelihood of treatment adherence, as clients are more likely to engage with approaches that align with their understanding of their problems.
Remember that insight-building is an essential aspect of psychotherapy that helps clients better understand themselves, their experiences, and their relationships [6]. By taking time to ensure shared understanding, you're laying groundwork for the client to develop actionable solutions based on a deeper self-awareness.
Avoid clinical jargon that may alienate the client
Despite clinicians acknowledging the importance of avoiding medical jargon when communicating with patients, its use in clinical settings remains common. Unfortunately, this technical language can create unnecessary barriers between you and your client.
A mixed-methods study revealed that an overwhelming 91% of survey respondents preferred doctors who communicated without medical jargon. Moreover, respondents described jargon-using healthcare providers as causing confusion, being too technical, uncaring, and condescending. Conversely, providers who used jargon-free language were perceived as good communicators, caring, empathetic, and approachable.
When translating clinical concepts for clients, consider replacing terms like:
"Ambulate" with "walk"
"Erythematous" with "red"
"Cognitions" with "thoughts"
"Affect" with "feelings"
"Psychosocial stressors" with "life challenges"
Even seemingly straightforward clinical observations can be misinterpreted. For instance, a casual remark like "Your potassium is up today" might make a patient think they should avoid eating bananas. Similarly, therapy jargon such as "I need to hold space for myself" can sound formal and distant compared to simply saying, "I'm feeling overwhelmed and need time to think".
The consequences of poor communication extend beyond momentary confusion. When clients don't understand what you're saying, they may:
Feel disrespected or mistreated
Experience frustration and diminished trust
Turn to unreliable sources like Google for answers
Miss important information about their condition
Become less engaged in the therapeutic process
The negative impact of jargon becomes particularly evident when delivering serious news or explaining next steps. In these moments, clients may lack the emotional bandwidth to absorb technical explanations. Slow down during these conversations and confirm the client is tracking each part of your discussion.
Interestingly, research found varied reasons why healthcare practitioners use jargon. The two most common explanations relate to what researchers call "jargon oblivion" - where clinicians either forget to switch from professional terminology to patient-friendly language or mistakenly believe patients understand terms they actually don't. Additionally, more than a third of respondents believed clinicians use jargon because they are poor communicators, want to make themselves feel important, or lack empathy.
By consciously avoiding jargon and translating complex ideas into accessible language, you demonstrate respect for your client while enhancing their understanding. This approach fosters a stronger therapeutic alliance and empowers clients to participate more fully in their own care.
As you conclude this first session, your client should leave with much more than a diagnosis. They should have a narrative that makes sense of their experiences, expressed in language they connect with emotionally. This shared understanding forms the foundation for everything that follows in therapy. With this crucial first step complete, you're ready to move to the second session, where you'll define starting points and direction for treatment.
Session 2: Define the Starting Point and Direction
After establishing a shared understanding of the client's situation in your first session, the second session focuses on defining measurable starting points and directions for therapy. Recent research indicates that determining treatment goals is an essential component of the decision-making process, although many practitioners receive little structured training in goal-setting techniques [7]. This session provides the framework for tracking progress and setting clear expectations.
Use scaling questions to assess current state
Scaling questions serve as powerful tools to quantify abstract concepts and create measurable baselines for therapy. Often described as the "workhorses" of solution-focused approaches, these questions ask clients to rate their situation on a standardized scale, typically from 1 to 10, with 1 representing the worst possible scenario and 10 representing the best [8].
The value of scaling questions extends beyond simple measurement:
They transform intangible experiences into concrete numbers
They help clients visualize their current state clearly
They create a reference point for measuring future progress
They allow exploration of the client's motivation and sense of control
When implementing scaling questions in your practice, consider this approach:
"On a scale from 0 to 10, where 0 represents zero success and 10 represents total success, what number would you give your current situation?"
Following this initial question, you can deepen understanding by asking:
"What tells you that you're at a 4 and not a 3?"
"What would need to happen for you to move up just one point on the scale?"
"When was the last time you were one point higher? What was different then?"
This technique not only provides quantifiable data but consequently helps clients recognize their existing strengths and resources. Research suggests that success scaling raises people's expectations and increases their determination to achieve success [9]. Indeed, studies have found that asking students to write about successful experiences led to higher expectations for future performance [9].
Throughout this process, remember that scaling questions work best when they help clients focus on possibilities rather than problems. They should orient toward the future while acknowledging the present reality.
Identify behavioral anchors for progress
Alongside numerical scales, behavioral anchors provide concrete reference points that make progress tangible and observable. These anchors are specific behaviors or observable indicators that correspond to different points on a scale, transforming abstract ratings into real-world actions and experiences.
Research demonstrates that behavioral anchors enhance the precision of assessments. The Adolescent Community Reinforcement Approach (A-CRA), for instance, uses specific behavioral anchors throughout its 73 procedure components, with detailed rating criteria for each point on its scales [10]. This specificity allows both therapists and clients to identify exactly what behaviors constitute progress.
To develop effective behavioral anchors:
Ask the client to describe what they would be doing differently at each level of the scale
Focus on observable actions rather than feelings or thoughts
Include both the presence of positive behaviors and the absence of problematic ones
Consider multiple life domains (work, relationships, self-care)
For example, if a client rates their anxiety at a 7, you might establish these behavioral anchors:
Moving to a 6: "I will attend one social gathering without leaving early"
Moving to a 5: "I will speak up in at least one meeting at work"
Moving to a 4: "I will reduce my checking behaviors to twice daily instead of hourly"
Essentially, behavioral anchors transform abstract goals into concrete actions that clients can take and that both of you can observe. This approach aligns with evidence suggesting that breaking actions into smaller manageable steps, with encouragement from practitioners, helps validate that goals are achievable [11].
According to recent research, youth advisors have identified that having goals broken down into manageable steps is one of the most helpful aspects of therapeutic goal-setting [12]. This process allows clients to experience early wins, building confidence and momentum toward larger goals.
Set S.M.A.R.T. goals collaboratively
Once you've established the current state through scaling and identified behavioral anchors, the next step involves setting structured goals using the S.M.A.R.T. framework. This widely-used approach ensures that goals are Specific, Measurable, Achievable, Relevant, and Time-bound [7].
Studies show that medical students trained to use SMART criteria had significantly higher scores for setting treatment goals (68.5%) compared to those using other approaches or no specific framework (29.6% and 30.8%, respectively) [7]. Additionally, the SMART group demonstrated better treatment monitoring (34.2% versus 19.3% and 24.6%) [7].
Let's examine each component:
Specific: Goals should answer the what, why, and how of objectives. Replace vague aspirations like "feel better" with specific intentions such as "practice mindfulness for 10 minutes daily to reduce anxiety symptoms" [13].
Measurable: Quantify progress whenever possible. Instead of "improve my relationships," try "have two meaningful conversations with my partner each week without raising my voice" [13].
Achievable: Goals must balance ambition with reality. Youth advisors have emphasized that ensuring goals are achievable is key to building good therapeutic relationships and addressing anxiety/depression effectively [11].
Relevant: Goals should align with the client's values and broader life objectives. Research indicates that collaborative goal setting enables genuine disclosures not otherwise possible and facilitates mutual support [11].
Time-bound: Adding timeframes creates urgency and focus. For example: "reduce panic attacks from daily to twice weekly within the next three months".
The process of setting SMART goals should be genuinely collaborative. Studies suggest that goal setting is most effective when it's a joint effort that respects the client's values, priorities, and motivations. This collaboration fosters stronger therapeutic alliances and increases client engagement in their own growth process.
Throughout goal setting, maintain awareness of potential barriers. Some clients may associate goals with negative past experiences, or face challenges like hopelessness, high distress levels, overthinking, or perfectionism [12]. Youth advisors have noted that in their experience, not all therapy contexts or types are equally conducive to goal setting [12].
Naturally, the language you use matters significantly. Research has found that youth advisors associate 'goals' with school/work contexts, while 'therapeutic goals' carried more personal and significant meanings [12]. Be attentive to terminology and adapt your language to resonate with each client's preferences.
Clarify what success looks like for the client
The final crucial step in this second session involves establishing a clear, shared vision of what constitutes success from the client's perspective. Evidence indicates that measuring progress in mental health treatment is essential because it allows for objective assessment of interventions and determines whether more intensive or different treatments might be necessary [15].
Yet the definition of success in therapy is highly individual. While traditional assessment tools often focus narrowly on symptom reduction, research shows that therapists consider three primary criteria for measuring quality of care: improvement in client functioning (56%), reduction of client's symptoms (42%), and the strength of the client-therapist relationship (42%) [16].
Notably, a majority of therapists surveyed (56%) indicated that functional improvement—not merely symptom reduction—was the most important signal of effective therapy [16]. This suggests that success measures should extend beyond clinical symptoms to include quality of life dimensions.
To help clients articulate what success looks like for them, consider exploring:
Their vision of daily life once therapy goals are achieved
The specific behaviors they would engage in
How others would notice they've changed
What would disappear or diminish in their experience
What would appear or increase in their experience
Solution-focused approaches often use future-oriented questions like: "Let's say that while you are sleeping tonight a miracle occurs and your problem has disappeared. How would you notice that the problem was gone? What would you be doing differently? What would other people notice as different about you?" [8]
This process of defining success should account for multiple dimensions. The OECD guidelines for measuring subjective well-being include questions in three areas: life evaluation (cognitive impression of life quality), affect (how people feel at given points), and eudaimonia (contentment, sense of meaning and purpose) [17].
Understanding success in these various dimensions allows for more comprehensive goal setting. On the individual level, people who score high on subjective well-being are likely to live longer, perform better in the workplace, and have lower health-care costs [17]. This underscores the importance of defining success broadly, beyond mere symptom reduction.
Before concluding this session, it's valuable to discuss how success will be monitored. Regular progress assessment helps identify patterns of change, which can help clinicians develop more efficient and effective treatment plans [15]. Transparent discussion about measurement methods builds trust and keeps both therapist and client accountable to the agreed-upon goals.
Remember that measuring progress isn't just about tracking outcomes—it's about building motivation. Research suggests that scaling questions boost clients' drive to reach their goals by helping them see progress, even when it feels slow [3]. As clients rate themselves higher on various scales over time, this visible movement forward can reinforce their commitment to the therapeutic process.
By the end of your second session, you and your client should have established clear starting points, identified concrete behavioral anchors, set SMART goals collaboratively, and defined what success will look like from the client's perspective. This shared understanding creates the foundation for the therapeutic contract and first actions that will be the focus of your third session.
Session 3: Create the Therapeutic Contract and First Action
The therapeutic contract represents the critical bridge between planning and action in your client's journey. Research shows that establishing this contract properly does more than just set administrative boundaries—it defines the reality of the therapeutic relationship itself and prepares the foundation for observing and modifying the client's psychic dynamics [4]. This third session transforms previous discussions into a formal agreement that will guide your work together.
Discuss roles and responsibilities explicitly
Clarifying roles and expectations at the outset prevents misunderstandings that could undermine treatment effectiveness. The therapeutic contract should explicitly outline the responsibilities of both you and your client, ensuring transparency and establishing the foundation for a productive alliance [18].
Initially, explain your role as the mental health professional. Psychologists in healthcare settings play several key functions:
Conducting clinical assessments using psychological tests and measurements
Providing interventions for individuals with physical and mental health challenges
Using specialized techniques to address emotional conflicts, personality disturbances, and skill deficits [19]
Subsequently, articulate the client's role as an active participant in the healing process. Unlike passive medical treatments, therapy requires engagement between sessions. Research indicates that a collaborative partnership characterized by mutual trust, respect, and understanding creates a non-judgmental space that fosters open communication [20].
Prior to moving forward, check that the client understands and accepts these responsibilities. You might say: "My role is to provide expertise and guidance, while your role involves trying new approaches between our sessions and providing honest feedback about what's working. Does this division of responsibilities make sense to you?"
Introduce a small behavioral experiment
Behavioral experiments serve as powerful tools to test the reality of clients' beliefs [21]. Introducing a small experiment in this third session accomplishes two important objectives:
It signals a shift from assessment to active treatment
It provides an early opportunity for success that builds momentum
When developing a behavioral experiment, ensure it directly addresses the client's core concerns while remaining manageable. The experiment should target a specific belief or thought pattern identified in your previous sessions [21].
Collaborate with your client through this process:
Identify the exact belief the experiment will target
Brainstorm ideas for the experiment together
Predict outcomes and devise a recording method
Anticipate challenges and develop solutions [21]
For instance, if a client experiences social anxiety and believes others will judge them harshly, you might design an experiment where they initiate a brief conversation with a store clerk while noting any actual negative reactions. This provides concrete evidence that can challenge distorted beliefs.
Research demonstrates that these experiments are not merely abstract exercises—they're powerful learning experiences. One practitioner reported a client who believed social settings without alcohol would cause extreme anxiety. Through a simple coffee meeting experiment, the client discovered his prediction of extreme nervousness didn't materialize as expected [6].
Gain informed consent for the treatment plan
Informed consent represents more than a legal requirement—it's an ethical cornerstone of psychological practice. The American Psychological Association emphasizes that psychologists must obtain informed consent using language reasonably understandable to clients [22].
The informed consent process should be ongoing rather than a one-time event, beginning with the first visit and revisited regularly [23]. Through this process, ensure your client understands:
The nature and objectives of therapy
Potential risks and benefits of treatment
Alternative approaches available
Limits of confidentiality
Roles and responsibilities of each participant [22]
Regarding treatment modifications, research suggests incorporating a general clause in your informed consent that allows for flexibility. This clause might state that you "reserve the right to digress from initial treatment goals when deemed clinically necessary" [24]. This provides flexibility while maintaining transparency.
To verify understanding, ask clients to summarize key points in their own words. For example: "To make sure I've explained everything clearly, could you tell me your understanding of how we'll be working together?"
Throughout this process, emphasize that informed consent remains a mutual, ongoing agreement between you and your client [24]. If treatment goals shift significantly, consider repeating or updating the consent process to ensure continued alignment.
Document the agreement and next steps
Proper documentation serves multiple purposes: it creates clarity, meets legal requirements, and establishes accountability. A well-documented therapeutic contract includes several essential elements:
Demographic/identifying information (client name, date of birth)
Session details (date, start/end times)
Your name and professional signature
Location information for telehealth sessions
Additionally, progress notes should document:
The client's presentation (mood, affect, appearance)
Relevant symptoms reported and observed
Treatment modalities used
The client's response to interventions
Progress toward established goals
Plans following the session
Remember that these notes may be requested by clients or even subpoenaed in legal proceedings. Therefore, ensure they remain primarily objective and respect client privacy. One therapist's example of documenting a plan in progress notes reads: "Client has committed to resuming a sleep schedule, beginning tonight, and agreed to turn off his smartphone an hour before the established 11PM bedtime".
Beyond formal documentation, provide clients with clear next steps. This creates momentum and prevents the loss of progress between sessions. These next steps should directly connect to the small behavioral experiment you've designed together.
Address potential risks of misalignment early
Misalignment between therapist and client can significantly undermine treatment effectiveness. Research highlights that aligning therapy with client motivations and expectations is key to building strong therapeutic relationships and enabling real progress [20].
Chiefly, be alert for signs of misalignment, which may include:
Reluctance to engage with homework or experiments
Consistently missing appointments
Passive participation during sessions
Disagreement about treatment priorities
In conjunction with addressing these signs, it's vital to have explicit conversations about potential obstacles. The contract should outline cancelation policies, financial obligations, and other logistical details that might otherwise create friction [18].
If misalignment occurs around treatment goals, psychologists face an ethical dilemma. The American Psychological Association's ethics code requires psychologists to "accept appropriate responsibility for their behavior" [22] while also respecting client autonomy. This balancing act demands careful consideration when treatment priorities differ.
In cases where clients hold potentially harmful beliefs, research suggests therapists may need to address these directly, even if doing so diverges from initial treatment goals [24]. For example, one case study described a therapist who needed to address a client's distorted beliefs about sexual consent, stating: "I want to shift our treatment focus and talk a little bit about how sexual consent is defined. This conversation could bring up some uncomfortable feelings, and we can stop talking about it at any time. Is that ok with you?" [24].
By proactively establishing processes for addressing disagreements, you create a framework that can withstand the inevitable challenges of the therapeutic journey. This third session creates not just a contract but a living agreement that will evolve as your therapeutic relationship develops.
With the foundation of shared understanding, clear goals, and explicit agreements in place, you and your client are now positioned to begin the real work of therapy. The initial three-session protocol transforms assessment into meaningful therapeutic momentum, setting the stage for sustainable change.
Conclusion
Establishing a structured approach after client assessment fundamentally changes how treatment unfolds. This 3-session protocol transforms clinical insights into meaningful therapeutic work rather than rushing prematurely into interventions. The protocol serves as a bridge between assessment and treatment, ensuring clients become active participants in their healing journey rather than passive recipients of therapy.
Session one builds the essential foundation through a shared case formulation, where you translate clinical concepts into accessible language and powerful metaphors. This collaborative understanding creates immediate resonance with clients, consequently increasing their engagement from the beginning. Session two defines clear starting points using scaling questions and behavioral anchors, thus establishing measurable targets that make progress tangible. Session three formalizes the therapeutic contract while introducing a small behavioral experiment, therefore shifting the relationship from planning to action.
The benefits of this deliberate approach extend beyond immediate client engagement. Clients who understand their diagnosis, actively participate in goal setting, and explicitly agree to treatment responsibilities show significantly higher rates of treatment adherence. Additionally, this protocol helps prevent common therapeutic pitfalls such as misalignment, poor engagement, and early dropout.
Remember that rushing into interventions without this foundational work often leads to disconnection between your clinical understanding and your client's experience. Conversely, taking time to build shared understanding, establish clear goals, and create explicit agreements sets the stage for sustainable change. This intentional beginning transforms diagnosis from a clinical label into a collaborative journey toward healing.
Through consistent application of this 3-session protocol, you create not just better treatment outcomes but also stronger therapeutic alliances. The time invested upfront pays dividends throughout the entire treatment process. Undoubtedly, these first steps after assessment might represent the most crucial phase of therapy—the bridge that transforms clinical insights into therapeutic momentum.
Key Takeaways
This structured 3-session protocol transforms post-assessment chaos into therapeutic momentum by creating shared understanding, measurable goals, and clear agreements before diving into interventions.
• Build shared understanding first: Translate clinical diagnoses into client-friendly narratives using metaphors and accessible language to create collaborative case formulations that resonate emotionally.
• Establish measurable baselines: Use scaling questions (1-10) and behavioral anchors to quantify abstract concepts, creating concrete reference points for tracking progress.
• Set SMART goals collaboratively: Work together to create Specific, Measurable, Achievable, Relevant, and Time-bound objectives that align with the client's values and vision of success.
• Formalize the therapeutic contract: Explicitly discuss roles, responsibilities, and expectations while introducing a small behavioral experiment to shift from planning to action.
• Prevent common pitfalls early: Address potential misalignment, establish clear documentation, and create frameworks for handling disagreements before they undermine treatment effectiveness.
This deliberate approach prevents the "premature action" trap that leads to poor engagement and early dropout. Research shows clients who actively participate in goal-setting and understand their treatment plan demonstrate significantly higher adherence rates and better outcomes. The time invested in these foundational sessions creates stronger therapeutic alliances and sets the stage for sustainable change throughout the entire treatment process.
FAQs
What is the purpose of the 3-session protocol after assessment?
The 3-session protocol aims to transform clinical insights into therapeutic momentum by creating a shared understanding with the client, establishing measurable goals, and formalizing a therapeutic contract before starting interventions.
How does the first session help build a shared case formulation?
In the first session, the therapist translates clinical diagnoses into client-friendly narratives using metaphors and accessible language. This creates a collaborative understanding that resonates emotionally with the client, increasing engagement from the beginning.
What tools are used in the second session to define starting points?
The second session utilizes scaling questions (typically on a 1-10 scale) and behavioral anchors to quantify abstract concepts and create concrete reference points for tracking progress throughout therapy.
How are treatment goals set in this protocol?
Treatment goals are set collaboratively using the SMART framework, ensuring they are Specific, Measurable, Achievable, Relevant, and Time-bound. This approach aligns the goals with the client's values and vision of success.
What is included in the therapeutic contract discussed in the third session?
The therapeutic contract explicitly outlines roles, responsibilities, and expectations for both the therapist and client. It also introduces a small behavioral experiment to shift from planning to action and addresses potential risks of misalignment early in the treatment process.
References
[2] - https://pmc.ncbi.nlm.nih.gov/articles/PMC11303933/
[3] - https://www.universalcoachinstitute.com/scaling-questions/
[4] - https://istfp.org/the-therapeutic-contract-how-treatment-arrangements-determine-the-effectiveness-of-therapy/
[5] - https://www.bild.org.uk/wp-content/uploads/2020/07/An-introduction-to-psychological-formulation.pdf
[6] - https://practicetransformation.umn.edu/practice-tools/behavioral-experiments/
[7] - https://pmc.ncbi.nlm.nih.gov/articles/PMC4917792/
[8] - https://pmc.ncbi.nlm.nih.gov/articles/PMC10098109/
[9] - https://www.tandfonline.com/doi/full/10.1080/2372966X.2021.1942196
[10] - https://pmc.ncbi.nlm.nih.gov/articles/PMC4000045/
[11] - https://bmcpsychology.biomedcentral.com/articles/10.1186/s40359-022-00879-5
[12] - https://www.corc.uk.net/news-and-blogs/collaborative-goal-setting-what-works-for-whom-in-therapeutic-relationships/
[13] - https://growtherapy.com/blog/what-are-smart-goals-in-therapy/
[15] - https://www.nami.org/Blogs/NAMI-Blog/June-2023/Rethinking-How-We-Measure-Progress-in-Mental-Health-Treatment
[16] - https://helloalma.com/blog/how-therapists-measure-progress/
[17] - https://www.apa.org/monitor/2013/06/success
[18] - https://www.stresslesstherapist.com/therapy-contracts-101-the-8-non-negotiables-you-need-to-know/
[19] - https://pmc.ncbi.nlm.nih.gov/articles/PMC3410123/
[20] - https://thedecisionlab.com/big-problems/strengthening-therapeutic-relationships
[21] - https://www.verywellmind.com/how-to-perform-behavioral-experiments-4779864
[22] - https://www.apa.org/ethics/code
[23] - https://www.apaservices.org/practice/business/management/informed-consent
[24] - https://pmc.ncbi.nlm.nih.gov/articles/PMC6901722/
If you’re ready to spend less time on documentation and more on therapy, get started with a free trial today
Not medical advice. For informational use only.
Outline
More articles