The Play Prescription: Why Everyday Play Is the Most Underutilized Mental Health Intervention

Mar 19, 2026
Nine percent of preschoolers worldwide experience anxiety [10]. Yet the most accessible intervention sits right in front of you—everyday play happening in homes and playgrounds across your community. Non-therapeutic play encompasses the pretend games, outdoor exploration, and unstructured activities that children engage in naturally. These moments offer profound mental health benefits that most clinicians overlook.
The preschool years create a critical window for emotional development [10]. During this period, everyday play functions as prevention, building resilience before symptoms take hold. A comprehensive 2025 systematic review examined 33 studies to identify which play forms deliver the strongest benefits for reducing anxiety, aggression, and fear in young children.
The results challenge what many assume about effective mental health work. Meaningful intervention doesn't require clinical settings or specialized equipment. The evidence points to something simpler and more powerful.
This article translates research findings into practical guidance you can use immediately. You'll learn how to prescribe specific types of play to parents, integrate play-based approaches into your current practice, and recognize when everyday play provides sufficient support versus when specialized intervention becomes necessary.
Your clients already have access to this intervention. The question is whether you'll help them use it effectively.
The Evidence: What the 2025 Systematic Review Found
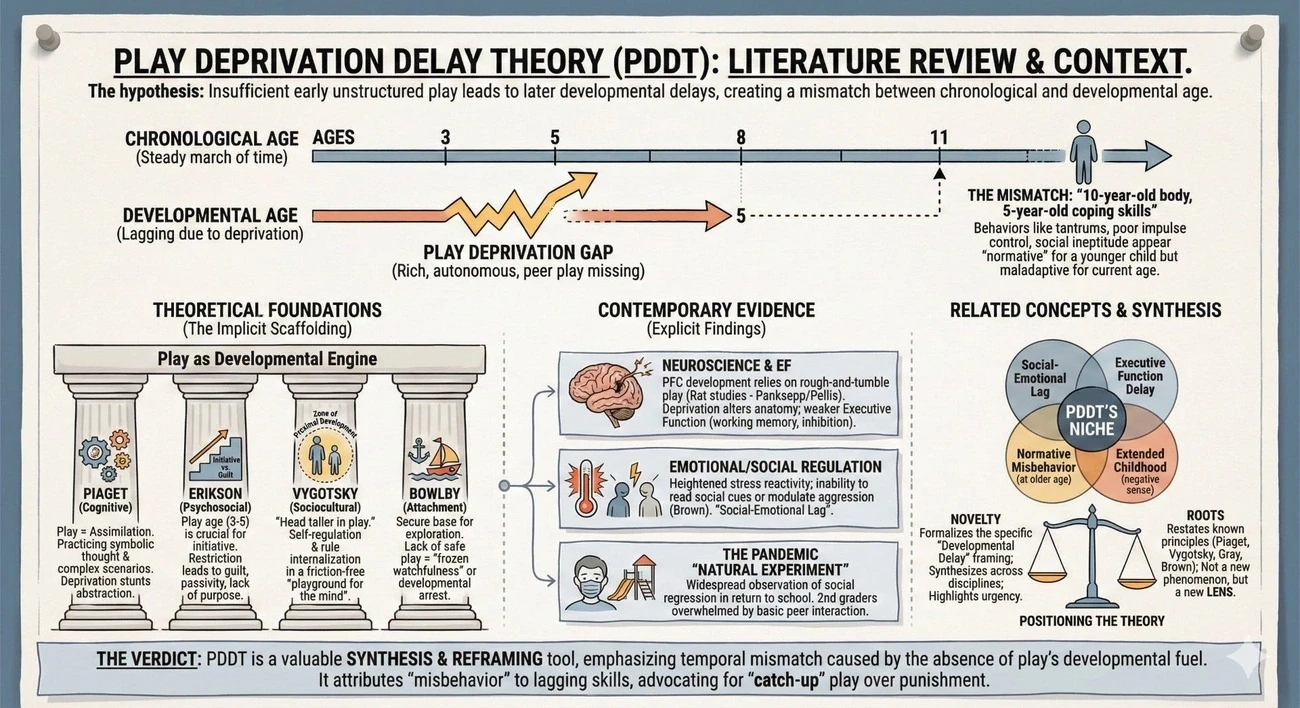
Image Source: Substack
The Scope of the Review
Researchers applied the PRISMA method to maintain scientific rigor throughout their analysis. Their systematic search covered three major databases: PubMed, ScienceDirect, and Scopus. Starting with 9,639 published articles from the past five years, the team narrowed their focus to 33 studies that met strict qualitative analysis criteria [10].
The screening process deliberately excluded clinical interventions. Instead, researchers concentrated on non-therapeutic play occurring in natural environments—homes, schools, and playgrounds where children spend their daily lives. Four distinct play types received examination: pretend play, play with rules, digital play, and outdoor play. Each type underwent assessment for its effectiveness in addressing emotional symptoms and supporting mental health outcomes in preschool-aged children [10].
This comprehensive approach matters because previous research remained fragmented across multiple disciplines. Developmental psychology, pediatric mental health, and educational research each contributed pieces of the puzzle, but no single study had connected these findings systematically. The five-year timeframe proves particularly valuable, capturing recent shifts in how children play, including increased screen exposure and reduced outdoor activity that directly affects your current client population.
The Key Finding: Pretend Play as the Gold Standard
Pretend play demonstrated the greatest corrective and developmental potential among all play forms examined [10]. The difference wasn't subtle—while every play type showed measurable benefits, pretend play distinguished itself through the breadth of mechanisms it activates simultaneously. Children who assign roles, negotiate scenarios, and construct narratives engage cognitive, emotional, and social processes that other play forms address only partially.
Supporting research reinforces these findings across multiple contexts. A meta-analytic study examining 43 independent studies with 2,614 participants found that play therapy produced a large-to-very-large overall effect size (g = 1.12, 95% CI [.94, 1.31]) on children's developmental outcomes [11]. Affective outcomes showed the largest effects, with early childhood participants benefiting most [11]. Additional systematic review data from children with cancer demonstrated that play interventions reduced depressive symptoms, stress, and anxiety, with a standardized mean difference for anxiety of -0.36 (95% CI -0.68, -0.03) favoring play therapy [12].
The connection between play and psychological health appears even more pronounced in school-aged populations. Research examining play performance revealed that executive functioning during play showed the strongest correlations with externalizing symptoms and prosocial behavior (rho = 0.311–0.620) [13]. Children with non-typical play patterns were 10 times more likely to display high psychosocial difficulties, and play performance factors explained nearly half the variance in psychosocial problems (adjusted R² = 0.477) [13].
Why This Matters for Clinical Practice
These findings fundamentally reframe early intervention approaches. Non-therapeutic play serves as an effective method to improve emotional intelligence and its components while decreasing anxiety, aggression, and fear [10]. The play happening in your clients' homes right now carries measurable mental health impact. Rather than asking parents to add new activities, you're helping them recognize and enhance existing opportunities.
Effect sizes documented across multiple reviews suggest that play interventions perform comparably to other evidence-based approaches for early childhood emotional regulation. When you recommend play, you're prescribing an intervention with substantial empirical support, not offering a gentle alternative to established treatment methods. The executive functioning data holds particular clinical significance because it indicates that play's cognitive demands directly strengthen neural systems responsible for self-regulation.
The Seven Generalized Mechanisms of Play
Cultural-historical research identified seven generalized mechanisms through which play enhances children's mental well-being and promotes development [10]. These mechanisms explain pretend play's superior performance: it engages all seven simultaneously.
Play creates a space where children process personal meanings and experiences. It provides opportunities to develop self-regulation skills through managing impulses within play scenarios. Play facilitates interactions with peers and adults in low-stakes contexts where mistakes carry no real-world consequences. It allows emotional expression and exploration without requiring direct confrontation of difficult feelings. Play builds cognitive flexibility through role-switching and scenario-building. It develops social cognition as children interpret others' intentions and adjust their behavior accordingly. Play offers a controlled environment for practicing problem-solving strategies that transfer to non-play contexts [10].
Understanding these mechanisms allows you to move beyond general encouragement toward specific clinical guidance. When parents question why pretend play matters more than educational applications, you can explain that pretend play activates all seven therapeutic systems while digital play typically engages only two or three.
Types of Play: What Works and Why

Image Source: Children's Medical Centers of Fresno
Each play type creates distinct pathways for emotional development. Understanding these differences helps you match interventions to specific therapeutic goals.
Pretend Play — The Gold Standard
Watch a two-year-old feed a stuffed bear with an empty spoon. She's building the foundation for complex emotional regulation. Around age three, this evolves into symbolic play—boxes become cribs, blocks transform into purring cats, empty bowls nourish invisible friends [13]. The high season arrives between ages three and five, when children construct elaborate narratives and negotiate complex role-play scenarios with peers [13].
This progression matters because pretend play strengthens executive function, language development, and perspective-taking abilities [13]. When children declare "I am the mom, you are the baby" and establish rules like "the baby can't drive the car," they practice the same cognitive flexibility that formal therapy targets. The child comforting a "sad baby" rehearses emotional attunement in a safe environment.
Research consistently demonstrates that play-based preschool curricula outperform direct instruction approaches in long-term academic outcomes and school engagement [13]. While structured teaching yields immediate gains, play-based learning builds lasting foundations for learning and social connection.
Play with Rules — Learning Self-Regulation
Games with rules create natural laboratories for self-control development during the critical ages of three to five [12]. Matching games require children to hold multiple items in working memory while following specific constraints—turn over only two tiles, remember their locations, resist the urge to peek [12]. "Red Light, Green Light" and "Freeze Dance" teach body regulation and emotional transitions between excitement and stillness [12].
Different games target specific regulatory skills. Pattern-matching activities challenge children to override automatic responses—ignoring size or color to find true matches [12]. This builds rule-switching abilities that develop gradually through the preschool years. Cooperative games offer particular value for children who struggle with frustration, removing competitive pressure while maintaining engagement and challenge [12].
Outdoor Play — Natural Stress Medicine
Data from 69,571 preschoolers reveals outdoor play's protective power. Children who spent time outside less than once weekly showed 2.55 times higher odds of anxiety symptoms compared to those outdoors seven or more times weekly [6]. The risk increased to 3.10 times higher for toddlers aged 1-3 years [6]. Duration matters too—children outdoors less than 30 minutes per session faced significantly higher anxiety risk than those spending 120 minutes or more outside [6].
Nature exposure delivers benefits that extend beyond physical activity [7]. Green spaces enhance cognitive development in children and improve attentional functioning in adults [7]. Stress levels drop within minutes of outdoor exposure for both children and adults [8]. Whether explained by biophilia, attention restoration, or stress reduction theories, the clinical message remains clear: outdoor time functions as medicine for early anxiety and irritability.
Digital Play — Balanced Approach Required
Screen time research presents a complex picture. A meta-analysis of 117 studies covering 292,000 children found that excessive screen time increases emotional and behavioral problems, particularly for children ages 6-10 compared to younger children [9][9]. Gaming carries higher risks than educational or recreational screen use [9].
The relationship follows a U-shaped curve—both no use and excessive use harm wellbeing, while moderate use can provide small benefits [1]. Well-designed digital games foster competence through mastery, agency through choice, and connection through collaboration [10]. A 10-week intervention in South Africa showed particular benefits for children experiencing loneliness or social isolation [10].
Digital play differs from passive screen consumption. When intentionally selected and balanced with physical and pretend play, it offers genuine developmental benefits without the risks associated with excessive screen exposure.
Clinical Implications: How to Prescribe Play

Image Source: AAP
Clinical Implications: How to Prescribe Play
You already know the evidence. Now you need practical steps to implement play-based interventions in your practice. This means changing how you discuss play with families—positioning it as essential medicine, not optional entertainment.
The Play Prescription Model
The American Academy of Pediatrics recommends that pediatricians educate families about the healing and protective powers of play [11]. This extends to all clinicians working with young children. The Prescription for Play program provides a structured approach: 15-minute provider training on play's developmental role, followed by integration into regular visits for children ages 18-36 months [12]. Providers distribute play kits with age-appropriate materials while modeling play techniques in real time [13].
The approach centers on literal prescriptions. Give caregivers specific instructions to play daily with their child [13]. Follow up at subsequent visits, continuing conversations about play's importance and building caregivers' capacity for consistent implementation [13]. A pilot study with eight providers found that all reported changes in how they introduced play discussions with pediatric families [12]. One provider noted it served as a reminder to discuss development through play [12].
Mental health clinicians can incorporate play guidance into initial assessments and ongoing treatment plans. Occupational therapy guidelines emphasize using play in both assessment and intervention, evaluating play participation as a meaningful outcome [14]. Most effective interventions match play activities to the child's interests and developmental level [15]. Guided or semi-structured play involving adults appears most frequently in research, often including peers as play partners [15].
What to Say to Parents
"When your child engages in pretend play, they're practicing emotional regulation and perspective-taking. This supports their mental health the same way exercise supports physical health."
Be specific: "I'm prescribing 20 minutes of unstructured pretend play each day. Follow your child's lead without directing the activity."
Parents need permission to prioritize play over structured activities. The Prescription for Play program helped caregivers understand how critical high-quality play is and how to implement it effectively [12]. One caregiver shared that the program removed her son's negative perspective about doctor visits, making them feel more supportive [12].
Screening for Play: What to Look For
Ask direct questions during assessments:
How does your child play?
Do they enjoy pretend scenarios?
How much unstructured outdoor time occurs daily?
Does your child have peer play opportunities?
Watch for red flags: inability to engage in pretend play by age four, rigid or repetitive play without variation, aggression during play that cannot be redirected, withdrawal from peer or adult play, and play consistently reenacting traumatic events without resolution. Play performance factors in school-aged children explained nearly half the variance in psychosocial problems, with children displaying non-typical play patterns being 10 times more likely to show high psychosocial difficulties.
When to Intervene
Everyday play works for most children as prevention. Refer for play therapy or further assessment when:
Play is consistently absent, rigid, or harmful
Emotional or behavioral symptoms persist despite adequate play opportunities
Play consistently ends in conflict or distress
The child shows developmental delay or social difficulty signs
Play therapy serves children ages 3-12 with emotional, behavioral, relational, or learning difficulties, or those who experienced traumatic or stressful experiences [16]. The intervention provides a trained clinician who observes play patterns therapeutically, creates a safe exploration space, employs structured techniques beyond everyday play, and guides parents on supporting play at home.
Prevention Focus: Building Resilience Before Symptoms Emerge

Image Source: Harvard Graduate School of Education - Harvard University
Prevention works better than treatment. This principle drives modern healthcare, yet mental health professionals rarely apply it to early childhood emotional development. Play-based prevention offers a different path forward.
Play as Primary Prevention
Children who play regularly with parents show lower rates of anxiety, depression, aggression, and sleep problems [17]. The protective effect reaches beyond immediate symptom relief. Play creates a buffer against stress, allowing children to process difficult emotions while feeling safe [17]. When a four-year-old recreates a scary experience through doll play, they're building emotional resilience [17].
The HighScope Perry Preschool Study tracked at-risk children for decades [18]. Those who attended play-based classrooms outperformed peers from direct instruction programs across every measure that mattered. At age 27, the play-based group owned homes, maintained stable employment, and avoided the problems that plagued the comparison group: school dropout, arrests, welfare dependency, and incarceration [18].
Self-directed play environments interrupted generational cycles of disadvantage [18]. Children deprived of play show lasting deficits in resilience, self-control, and social connection. The implications for your practice are clear: prescribe play now to prevent problems later.
The Critical Window (Ages 3-7)
Brain development creates a narrow opportunity for intervention. Between 18 months and three years, neural connections multiply to reach 1,000 trillion—double the density found in adult brains [3]. Social-emotional systems, motor control, and language centers undergo rapid development [3]. Ages three to seven represent the optimal period for establishing emotional regulation patterns through play.
Pretend play emerges between 24 and 36 months as toddlers learn to suspend reality [3]. Symbolic thinking develops, enabling increasingly complex imaginative scenarios [3]. Three and four-year-olds create elaborate narratives featuring superhero battles, pirate adventures, and fairy kingdoms [19]. These stories require cognitive skills that strengthen executive functioning systems directly.

Guidance for Parents
Successful play-based prevention requires specific environmental conditions. Stock your child's space with open-ended materials: blocks, dress-up clothes, art supplies [2]. Create a designated play area free from distractions [2]. Limit screen time to encourage face-to-face interaction that builds social skills [2].
Participate by narrating your child's actions rather than directing them [2]. "You're making the bear very comfortable in that bed" supports language development and emotional expression without controlling the narrative.
Resist the urge to fill every moment with structured activities [20]. Boredom serves development by forcing children to plan, organize thoughts, and solve problems independently [20]. Allow minor risks and small failures during play [2]. These experiences teach experimentation and resilience.
Guidance for Schools
Schools hold significant power to protect or undermine children's mental health. The dramatic reduction in children's free play time during the 1980s coincided with rising rates of anxiety, depression, and suicide [21]. Today, 83% of teenagers identify school as their primary source of stress [21].
Educational leaders can reverse this trend through concrete policy changes: eliminate excessive testing for young children, guarantee full recess periods, extend lunch to a full hour, and avoid homework before middle school [21].
Play-based kindergartens featuring dramatic play, outdoor exploration, and child-led activities produce stronger social-emotional outcomes than academic-focused programs. Structured recess programs train adult facilitators to promote inclusive, cooperative play that reduces conflict. Teachers benefit from training in play observation to identify children who need additional support.
Your advocacy matters. Speak with school administrators about protecting play as a mental health intervention, not discretionary time subject to elimination when academic pressures mount.
Educational Applications: Play-Based Emotional Learning

Image Source: We Are Teachers
The State of Play in Schools
Kindergarten classrooms once buzzed with dramatic play centers and block areas. Today, worksheets and direct instruction dominate early childhood education [22]. The shift began in the 1990s when free play disappeared, replaced by rigid curricula focused on academic benchmarks [23]. This "schoolification" transformed kindergarten into first grade [23].
Change is happening. New Hampshire mandated play-based kindergarten in 2018, requiring child-directed experiences including movement, creative expression, and outdoor exploration [22]. Oklahoma followed with the Play to Learn Act in 2021, protecting play-based approaches through third grade [24]. Connecticut joined this movement in 2024, requiring play-based learning in all public early childhood programs [24].
These policy changes recognize what research demonstrates: guided play helps children master academic content while building executive function skills [24]. Children maintain agency in their learning while adults facilitate specific educational goals.
Models That Work: Culturally Adapted Play Programs
Effective play interventions reflect children's cultural backgrounds. Programs incorporating traditional games, local stories, and familiar materials increase engagement and learning outcomes [25]. Communities embrace these approaches more readily, creating supportive environments for implementation [25].
A study in Tamil Nadu incorporated traditional games like Paandi (hopscotch) and Paramapadham (snakes and ladders) into behavioral interventions [4]. Folk storytelling enhanced social understanding and emotional regulation [4]. Children showed increased motivation and better real-world social interactions when play activities connected to their cultural experiences [4]. These results demonstrate that culturally tailored approaches improve both utilization and effectiveness [4].
The principle extends beyond specific cultural contexts. Children engage more deeply when play connects to their lived experiences and family traditions.
What Clinicians Can Advocate For
Your voice carries weight in educational settings. Policy creates the foundation for protecting children's access to play [22]. Start conversations with school administrators about specific changes:
Protect recess as non-negotiable time. Frame it as a mental health intervention, not discretionary activity.
Establish play-based emotional learning programs. Recommend incorporating puppetry and role-play into existing curricula.
Provide teacher training in play observation. Help educators recognize when play patterns signal children need additional support.
Support state-level legislation that formalizes investment in play-based learning. Offer parent workshops explaining how play-based emotional learning benefits children's mental health. These educational efforts help families advocate effectively within their children's schools.
Your clinical expertise strengthens the case for play in educational settings. Schools need this guidance to create environments that support both learning and emotional development.
When Everyday Play Isn't Enough: The Role of Play Therapy

Image Source: Healthline
Understanding the Difference
Play therapy operates through systematic use of theoretical models, establishing an interpersonal process where trained therapists harness play's therapeutic powers to help clients prevent or resolve psychosocial difficulties and achieve optimal growth [26]. This approach differs fundamentally from the everyday play you've been prescribing.
Both involve toys and imagination. However, play therapy requires a licensed mental health practitioner trained specifically in child development and play therapy fundamentals [26]. These professionals create carefully designed playrooms with toys selected to promote emotional expression and represent various relationships, emotions, and situations [26]. Minimal rules allow children to explore emotions openly while therapists observe patterns and conceptualize what each child experiences [26].
Neuroscience explains why this distinction matters. Trauma effects reside in nonverbal brain areas including the hippocampus, amygdala, and brain stem, while communication ability resides in the frontal lobe [27]. Symbolic and role-play activities used in play therapy help move traumatic experiences from nonverbal brain regions to the frontal lobe [27].
Recognizing When to Refer
Children navigating difficult situations, childhood trauma, and adverse childhood experiences benefit from play therapy as an entry point for healing [26]. Consider referral for divorce, grief, illness, bullying, emotional or physical abuse, war, and persistent anxiety [26]. Children with behavioral or anger problems often need play therapy to learn regulating behaviors [26].
Ages 3-12 represent the optimal window, as this developmental stage uses play as a primary means of communication and expression [27].
Treatment Outcomes
Children engaging in child-centered play therapy demonstrate increased social-emotional wellness, improved academic performance, developed coping strategies and creative problem-solving skills, and improved relationships with caregivers and teachers [26].
Treatment typically spans 10-20 sessions lasting 45 minutes each [28]. Sessions may include only the child or involve parents when appropriate, with caregivers receiving guidance on reinforcing lessons at home [28].
Building Your Referral Framework
Everyday play functions as prevention. Play therapy serves as intervention when children have exhausted their own problem-solving tools [29]. Both remain essential components of your comprehensive mental health approach for young children.
Stay confident in your ability to determine when each approach serves your clients best.
Documentation: How to Capture Play-Based Work

Image Source: Renewing Hearts Play Therapy Training
Effective documentation elevates play-based interventions from casual observations to clinical evidence. Your notes must reflect play's therapeutic mechanisms while meeting professional standards.
Initial Assessment Documentation
Play-based assessments in natural settings provide accurate developmental information, particularly for children with delays or disabilities [30]. Early childhood professionals increasingly rely on authentic assessment tools including play-based evaluations, family interviews, and structured questionnaires [30]. Conduct these assessments in familiar environments—homes, childcare centers, libraries, and playgrounds—where children demonstrate typical behaviors [30].
Document specific play patterns you observe. Note the child's preferred play types, duration of engagement, and interaction styles with materials and people. Record any concerning behaviors such as rigid play sequences, inability to engage in pretend scenarios, or consistent withdrawal from peer interactions.
Prevention-Focused Progress Notes
Your documentation should capture concrete recommendations and parent responses. Record specific agreements: "Parents committed to 20 minutes daily unstructured pretend play" or "Family will prioritize 60 minutes outdoor time minimum." Include planned follow-up dates and specific topics for future discussions.
Track implementation progress across sessions. Note changes in play patterns, parent confidence levels, and any barriers to consistent play engagement at home.
Clinical Progress Documentation
Pediatric documentation requires adaptation of standard SOAP formatting [5]. Structure notes around the unique developmental needs of young clients [5]. Your theoretical orientation directly shapes note content—document observations through your chosen clinical lens [31].
Record specifics: which toys captured the child's attention, whether focus remained on single items or shifted between multiple materials, and how the child used objects symbolically [31]. Keep entries concise yet thorough [31].
Include direct quotes when possible. "Child stated 'The bear is scared like me'" provides richer clinical data than "Child expressed fear through play."
Quick Reference: Play Interventions at a Glance
Focus Area | What the Research Shows | How to Apply This | Who Benefits | Your Next Steps |
The Research Foundation | Pretend play delivers the strongest therapeutic benefits across 33 studies; Play therapy shows large effect sizes (g = 1.12); Seven therapeutic mechanisms work together; Children with atypical play patterns face 10x higher risk for difficulties | Position play as evidence-based medicine, not entertainment; Use pretend play as your go-to recommendation; Screen for play patterns in every assessment | Mental health clinicians, pediatricians, researchers | Start prescribing play today; Ask specific questions about play during intake; Recognize play's scientific validity |
The Four Play Types | Pretend play engages all therapeutic systems; Outdoor play under 30 minutes increases anxiety risk 2.55-3.10x; Rule-based games build self-regulation; Digital play works best in moderation | Match recommendations to specific goals; Prescribe 20+ minutes daily pretend play; Ensure 120+ minutes weekly outdoor time | Parents, clinicians, educators | Write specific play prescriptions; Emphasize outdoor time duration; Guide parents on play type selection |
Clinical Practice Integration | American Academy of Pediatrics recommends play education; Prescription for Play model shows provider behavior changes; Play assessment explains 47.7% of emotional problems | Frame discussions around play as medicine; Give literal prescriptions; Include play screening in standard assessments | Pediatricians, mental health professionals, OTs | Ask: "How does your child play?"; Watch for red flags: no pretend play by age 4, rigid patterns, persistent conflict; Document play recommendations clearly |
Prevention Approach | Regular parent-child play reduces anxiety, depression, aggression; HighScope Perry Study tracks 40+ year benefits; Brain development peaks ages 18 months-3 years with 1,000 trillion synapses | Build resilience before problems start; Protect unstructured time; Allow healthy boredom and minor setbacks | Parents, schools, policy makers | Recommend open-ended materials; Help parents resist over-scheduling; Advocate for protected recess time; Support play-friendly policies |
School Applications | New Hampshire, Oklahoma, Connecticut mandate play-based learning; Cultural adaptations increase engagement; Guided play enhances executive function | Advocate for play protection in educational settings; Support culturally relevant approaches; Train educators in play observation | School administrators, teachers, policy advocates | Protect recess as non-negotiable; Establish emotional learning through play; Provide teacher training; Support legislative efforts |
When to Refer | Play therapy serves ages 3-12 most effectively; Treatment typically requires 10-20 sessions; Trauma processing moves from nonverbal to verbal brain regions | Recognize everyday play limits; Understand specialized intervention timing; Maintain prevention-intervention continuum | Mental health clinicians, parents, play therapists | Refer when play is absent, rigid, or harmful; When symptoms persist despite adequate play; For trauma processing needs; Continue everyday play alongside therapy |
Documentation Methods | Play-based assessments provide more accurate developmental data; Natural settings yield better information; SOAP format adapts well to pediatric work | Document play recommendations with specificity; Use authentic assessment tools; Keep notes straightforward yet complete | Therapists, clinicians, early childhood specialists | Use play-based tools in natural environments; Document parent agreements and follow-up plans; Note specific toys and engagement patterns; Maintain theory-based observations |
Conclusion: The Most Underutilized Intervention
Pretend play represents the most powerful everyday intervention for building emotional resilience in young children. Your clinical approach can shift today.
Stop waiting for symptoms to develop. Start prescribing 20 minutes of daily unstructured pretend play as prevention. This isn't adding another task to overwhelmed families—you're helping them recognize the therapeutic value of what's already happening in their living rooms.
Screen for play patterns during every assessment. Guide parents to follow their child's lead rather than directing activities. Advocate for protected play time in educational settings. Document play recommendations with the same specificity you use for other evidence-based interventions.
When a four-year-old constructs elaborate tea party rules or negotiates superhero battle scenarios, they're practicing emotional regulation and perspective-taking. This is clinical work happening outside your office.
The research supports this approach. The families you serve need this guidance. Prescribe play with the same confidence you bring to other therapeutic recommendations.
Your clients already have access to this intervention. Help them use it effectively.
Key Takeaways
Research reveals that everyday play, particularly pretend play, functions as a powerful mental health intervention that clinicians are dramatically underutilizing for children ages 3-7.
• Pretend play outperforms all other play types - A 2025 systematic review of 33 studies found pretend play activates all seven therapeutic mechanisms simultaneously, making it the gold standard for emotional development.
• Prescribe play like medicine - The American Academy of Pediatrics recommends literally prescribing 20 minutes of daily unstructured pretend play to parents, framing it as prevention rather than entertainment.
• Outdoor time prevents anxiety - Children who spend less than 30 minutes outdoors per session show 2.55-3.10 times higher anxiety rates compared to those getting 120+ minutes daily.
• Screen for play patterns during assessments - Red flags include inability to engage in pretend play by age 4, rigid or repetitive play patterns, and play consistently ending in conflict or distress.
• Ages 3-7 represent the critical window - Brain synapses reach twice adult density during this period, making it optimal for building emotional regulation patterns through play-based interventions.
The research demonstrates that when children assign roles, negotiate scenarios, and construct narratives during pretend play, they're practicing the same emotional regulation and perspective-taking skills that formal therapy targets. This positions everyday play as both accessible prevention and evidence-based intervention that deserves clinical priority alongside traditional mental health approaches.
FAQs
At what age should children start engaging in pretend play for mental health benefits?
Children typically begin pretend play between 24 and 36 months when they develop the ability to suspend reality and engage in symbolic thinking. The optimal developmental window for building emotional regulation through play is ages 3-7, when brain synapses reach twice the density of adult brains. By age 3, children can create detailed narratives and engage in dramatic role-play, making this the ideal time to encourage daily unstructured pretend play sessions.
How much outdoor play time do children need to reduce anxiety symptoms?
Research shows that children who spend less than 30 minutes outdoors per session have significantly higher anxiety risk compared to those getting 120 minutes or more daily. Children aged 0-3 years who were outdoors less than once weekly had 2.55 to 3.10 times higher odds of developing anxiety symptoms compared to children who played outside seven or more times weekly. Outdoor exposure provides stress reduction benefits within minutes for both children and adults.
What are the warning signs that a child needs play therapy instead of just everyday play?
Red flags include inability to engage in pretend play by age 4, consistently rigid or repetitive play patterns without variation, play that always ends in conflict or distress, and persistent emotional or behavioral symptoms despite adequate play opportunities. Children who consistently reenact traumatic events through play without resolution, or who show developmental delays affecting social interaction, may benefit from specialized play therapy with a trained mental health professional.
How does pretend play specifically help with emotional regulation in young children?
Pretend play activates seven therapeutic mechanisms simultaneously: it allows children to process personal experiences, practice self-regulation by managing impulses within scenarios, develop social cognition through interpreting others' intentions, build cognitive flexibility through role-switching, and practice problem-solving in low-stakes contexts. When children assign roles and negotiate rules during imaginative play, they're strengthening the same neural systems responsible for emotional control that formal therapy targets.
Should parents be concerned about digital play and screen time for preschoolers?
Digital play shows a U-shaped relationship with mental health—both no use and excessive use negatively impact wellbeing, while moderate use can have small positive effects. Gaming is associated with higher risks compared to educational screen use, and older children (ages 6-10) are more vulnerable to developing socioemotional problems from excessive screen time. Well-designed digital games can foster competence and social connection when intentionally selected and balanced with physical and pretend play activities.
References
[1] - https://doi.org/10.3390/children12050551
[2] - https://pmc.ncbi.nlm.nih.gov/articles/PMC11924121/
[3] - https://ijonse.net/index.php/ijonse/article/view/7429
[4] - https://www.sciencedirect.com/science/article/pii/S2405844025020043
[5] - https://pmc.ncbi.nlm.nih.gov/articles/PMC9329709/
[6] - https://childmind.org/article/the-power-of-pretend-play-for-children/
[7] - https://www.fau.edu/newsdesk/articles/pretend-play-early-childhood
[8] - https://nurtureandthriveblog.com/my-favorite-games-for-self-regulation/
[9] - https://www.edparenting.com/blog/building-emotional-regulation-skills-through-play-and-connection
[10] - https://pmc.ncbi.nlm.nih.gov/articles/PMC12007297/
[11] - https://www.apa.org/monitor/2020/04/nurtured-nature
[12] - https://hsph.harvard.edu/news/time-spent-in-nature-can-boost-physical-and-mental-well-being/
[13] - https://www.apa.org/news/press/releases/2025/06/screen-time-problems-children
[14] - https://www.unicef.org/innocenti/documents/how-does-time-children-spend-using-digital-technology-impact-their-mental-well-being
[15] - https://joanganzcooneycenter.org/2024/04/30/can-digital-games-enhance-childrens-wellbeing/
[16] - https://www.psychologytoday.com/us/blog/worry-free-kids/201808/new-aap-report-recommends-prescription-play
[17] - https://www.weitzmaninstitute.org/wp-content/uploads/2023/10/AH_Lego-Issue-Brief-2023_0920-Final.pdf
[18] - https://pmc.ncbi.nlm.nih.gov/articles/PMC11776346/
[19] - https://www.rcot.co.uk/explore-resources/children-young-people-families/play-practice-guideline
[20] - https://apps.asha.org/EvidenceMaps/Articles/ArticleSummary/5e431227-e8c4-ed11-8145-005056834e2b
[21] - https://cbpt.org/directive-play-therapy/
[22] - https://www.unicef.org/parenting/child-development/how-play-strengthens-your-childs-mental-health
[23] - https://time.com/6696777/play-increases-resilience-essay/
[24] - https://www.maziply.com/blogs/blog/development-play-stages-of-play-and-why-it-matters?srsltid=AfmBOor7lYYE8uXgMYPtARaxo3LFiC-1_Izk8m4SVK54jvTn9GT3BFgc
[25] - https://www.beginlearning.com/parent-resources/pretend-play/
[26] - https://www.stepaheadaba.com/blog/how-to-reinforce-appropriate-play-skills-at-home
[27] - https://childcare.gov/consumer-education/support-my-childs-health-development/supporting-childrens-learning-through-play
[28] - https://www.gse.harvard.edu/ideas/edcast/24/02/improving-mental-health-through-independent-play
[29] - https://ies.ed.gov/learn/blog/prioritizing-play-importance-play-based-learning-early-education
[30] - https://www.naeyc.org/resources/pubs/yc/summer2022/power-playful-learning
[31] - https://www.brookings.edu/articles/tracking-the-winds-of-change-on-the-american-education-policy-landscape-the-emergence-of-play-based-learning-legislation-and-its-implications-for-the-classroom/
[32] - https://pmc.ncbi.nlm.nih.gov/articles/PMC12441714/
[33] - https://journals.lww.com/mhhb/fulltext/2025/07000/culturally_adapted_play_based_behavioral.4.aspx
[34] - https://gsehd.gwu.edu/child-centered-play-therapy
[35] - https://pmc.ncbi.nlm.nih.gov/articles/PMC10328142/
[36] - https://www.gillettechildrens.org/conditions-care/play-therapy
[37] - https://www.a4pt.org/page/PTMakesADifference/Play-Therapy-Makes-a-Difference.htm
[38] - https://pmc.ncbi.nlm.nih.gov/articles/PMC10072816/
[39] - https://www.blueprint.ai/blog/streamlining-documentation-for-therapists-example-soap-notes-for-children-and-adolescents
[40] - https://www.meehanmentalhealth.com/the-playful-therapist-blog/play-therapy-progress-note-tips
If you’re ready to spend less time on documentation and more on therapy, get started with a free trial today
Not medical advice. For informational use only.
Outline
More articles






