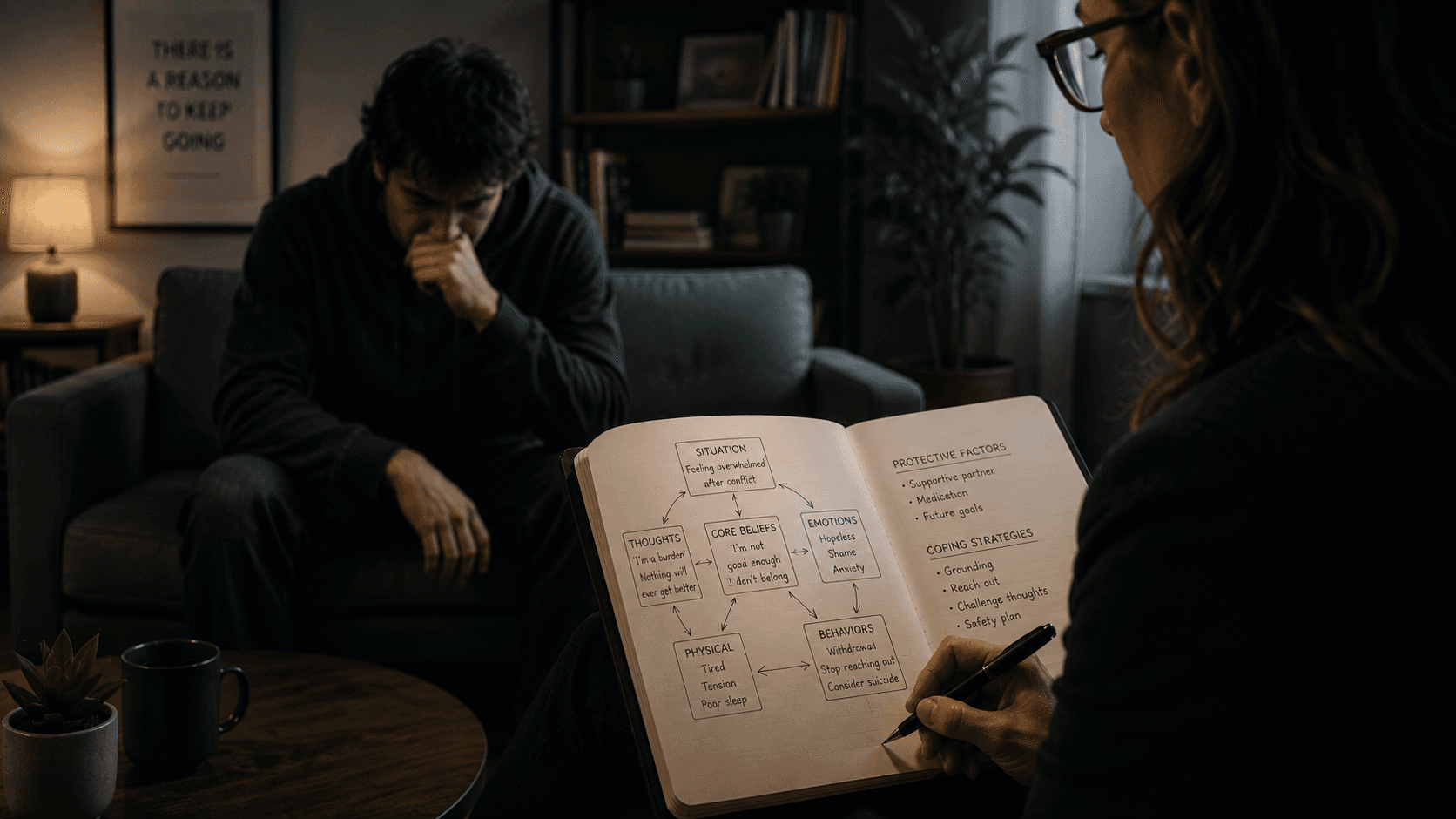
Understanding Unspecified Mood Disorder F39 in Pediatric Practice: Diagnostic Criteria for Children and Adolescents

Feb 24, 2026
Pediatric mood disorder diagnosis demands both clinical precision and developmental awareness. Children and adolescents rarely present with textbook symptoms. Instead of verbalized sadness, you'll encounter irritability, behavioral shifts, and physical complaints that mask underlying emotional distress.
The numbers tell a clear story. Between 2-5% of children and adolescents experience significant depression [14]. Girls face at least twice the risk of developing depression compared to boys [14]. These young patients deserve immediate attention, yet their developing brains resist premature diagnostic categorization.
F39 serves a specific clinical purpose in pediatric practice. This diagnostic code acknowledges mood disturbances that clearly impact functioning while the full clinical picture develops. Rather than forcing specificity where none exists, F39 provides the foundation for early intervention while maintaining diagnostic honesty.
This guide walks you through appropriate F39 documentation, real-world clinical scenarios, and practical strategies for family conversations. The goal remains simple: deliver effective treatment while respecting the developmental realities that make pediatric mood disorders uniquely challenging to diagnose and treat.
The Challenge of Mood Disorders in Developing Brains
Developmental Heterogeneity in Children and Adolescents
Brain development follows no universal timeline. A 12-year-old expressing mood dysregulation through irritability and oppositional behavior presents one clinical picture. That same symptom profile in a 16-year-old might signal emerging bipolar spectrum pathology. In an 8-year-old, it could indicate developmental trauma or early-onset depression.
The lifetime prevalence of mental, behavioral, and developmental disorders among children aged 3 to 17 years climbed from 25.3% to 27.7% between 2016 and 2021, with specific increases in anxiety, depression, learning disability, developmental delay, and speech or language disorder [14]. These conditions frequently co-occur and share risk and protective factors [14]. Complex clinical presentations emerge that resist straightforward categorization.
Despite increasing recognition, diagnostic precision proves elusive during initial presentations. Each year from 2016 to 2021, approximately 60% of children with mental, behavioral, and developmental disorders received mental or developmental services in the past 12 months [14]. Yet the developmental variability means symptoms may not fit established criteria at first encounter.
The Shifting Clinical Picture Over Time
Pediatric mood disorders evolve as moving targets. Recurrent episodes occur frequently in both depressive spectrum disorders (80%) and bipolar spectrum disorders (62.5%) [13]. High rates of progression from bipolar disorder-not otherwise specified or cyclothymic disorder to bipolar disorder type 1 or 2 have been documented [13].
Your initial evaluation may capture only a snapshot. The clinical picture you observe today may bear little resemblance to what emerges six months later. Research on childhood-onset depressive spectrum disorders shows that while many youth recover, sustaining remission proves difficult [13]. Treatment effects for pediatric mood disorders, while often enduring, tend to be non-specific to particular treatment modalities over the long term [13]. This suggests the underlying pathology itself remains fluid during developmental windows.
Somatic and Atypical Presentations in Youth
Physical symptoms often mask emotional distress in children. They express psychological pain through their bodies rather than words. Between 1988 and 2011, the percentage of boys with psychosomatic problems larger than the 90th percentile increased from 5.0% to 9.1%, and in girls from 16.7% to 24.5% [32].
The connection between physical and emotional symptoms runs deep. Up to 10.8% of children and adolescents suffer from a chronic somatic disorder and show a threefold increased risk of developing psychiatric comorbidities compared to healthy controls [32]. Somatic symptom disorders are equally common among young boys and girls but become more prevalent among adolescent girls than adolescent boys [32].
These presentations create diagnostic complexity. Up to 50% of children and adolescents with somatic symptom disorders suffer from psychiatric comorbidity [32], particularly anxious or depressive symptoms. Rather than verbalizing emotional pain, these young patients present with chronic pain, fatigue, headaches, and gastrointestinal complaints that lead to school absence, high socioeconomic costs, and frequent healthcare service use [32].
The Problem of Subthreshold Mood Conditions
Not all mood disturbances meet full diagnostic criteria, yet they still cause significant impairment. Between 1999-2002 and 2007-2010, the proportion of medical visits reporting not otherwise specified psychiatric diagnoses compared with full diagnostic criteria rose prominently for major mood diagnostic subtypes [11]. Among all visits for mood disorders, NOS visits grew proportionally 1.5-fold from 45.3% in the 1999-2002 period to 68.8% in the 2007-2010 period [11].
The increase proves particularly striking for bipolar disorder. NOS visits increased more than 18-fold, from 3.6% to 72.6% [11]. This surge reflects clinical reality: many young patients present with mood symptoms that don't fit neat diagnostic boxes.
Subthreshold presentations carry real risks. Adolescents with subthreshold depressive disorder face an estimated 67% risk for escalation to full-syndrome depressive disorders [2]. Children with subthreshold bipolar disorder, estimated to affect up to 6% of youth [2], demonstrate high rates of psychiatric comorbidity, functional impairment, and suicidality [2]. Adolescents with three or more risk factors (severity of depressive symptoms, medical conditions/symptoms, history of suicidal ideation, history of anxiety disorder, and familial loading for depression) had an estimated 90% chance of escalating to full-syndrome depressive disorder [2].
F39: What the Unspecified Mood Disorder Code Actually Means
Technical Definition and DSM-5 Criteria
The DSM-5-TR restored unspecified mood disorder after an unexpected gap. Originally, the mood disorders category was eliminated in favor of separate bipolar and depressive disorder classes, which inadvertently removed unspecified mood disorder as a diagnostic option [11]. Clinicians quickly identified this problem in their daily practice.
The restoration addresses a specific clinical reality: presentations where symptoms characteristic of a mood disorder cause clinically significant distress or impairment, but do not meet full criteria for any specific disorder, and where choosing between unspecified bipolar and unspecified depressive disorder proves difficult [37].
F39 fills a genuine clinical need. Use this code when you observe mood disturbances that resist categorization - symptoms that clearly suggest a mood disorder impacting functioning, yet the clinical picture remains ambiguous [13]. The category appears in both the depressive disorders and bipolar disorders chapters of the DSM-5-TR due to the absence of an overarching mood disorders grouping [11]. This dual placement makes DSM-5-TR more compatible with ICD-10-CM and ICD-11, which also include this category [11].
For pediatric practice, F39 offers particular value. The restoration provides clinicians with a more accurate and less stigma-prone diagnosis for mixed presentations [11]. Diagnostic pictures shift constantly with development, and F39 acknowledges current symptomatology without forcing premature specificity.
Clinical Validation Requirements for F39 Diagnosis
F39 demands thorough clinical validation, not diagnostic shortcuts. Your documentation must justify why an unspecified code is appropriate rather than reflecting incomplete assessment [32]. Insurance auditors focus specifically on verifying that documentation reflects an exhaustive assessment process [32].
Your records need specific elements: thorough patient history, clear description of mood disturbances, and explicit ruling out of more specific mood disorder categories [32]. The unspecified status must reflect genuine diagnostic uncertainty rather than superficial evaluation. Auditors examine detailed symptom documentation, differential diagnosis processes, and explanations of why more specific codes were not applicable [32].
Document your rationale for choosing F39 clearly. Include factors contributing to diagnostic uncertainty such as limited information, complex symptoms, or atypical presentation [14]. Your clinical notes should reflect steps taken to exclude more specific diagnoses, underlying conditions that obscure full assessment, and plans for follow-up evaluations [32]. This documentation approach aligns with professional standards while reducing audit risks.
F39 remains billable for reimbursement purposes [31]. Payers expect periodic justification for maintaining unspecified codes over time, so your documentation should support ongoing clinical reasoning as cases evolve.
What F39 Is Not: Common Misconceptions
F39 is not a shortcut for insufficient workup. This diagnostic code requires comprehensive evaluation to justify its use. Some clinicians default to unspecified codes when a more specific diagnosis is actually possible, leading to inadequate treatment planning [14]. This approach undermines the code's legitimate clinical purpose.
F39 operates differently from specific codes like F31 (bipolar disorder) or F33 (major depressive disorder, recurrent) in terms of diagnostic certainty [14]. Those codes align clearly with established criteria, while F39 indicates ambiguity requiring further evaluation and ongoing monitoring [14]. Unspecified diagnoses apply when symptoms fit within a broader category but don't meet full criteria for a more specific disorder [14].
Avoid F39 when symptoms arise solely from medical conditions, substance effects, or trauma without clear mood disorder features [14]. These presentations may fit better in adjustment disorders or other diagnostic categories. The unspecified mood disorder designation captures affective symptoms that impact emotional well-being but don't meet strict criteria for other specified mood disorders [13].
Most importantly, avoid using F39 as a permanent diagnosis. Emergency room settings may use F39 when insufficient information exists for more specific diagnosis [11], but outpatient clinicians working longitudinally with pediatric patients should view F39 as a working diagnosis requiring active reassessment. It serves as a starting point during diagnostic evolution, not a final destination.
The Case for F39 in Pediatric Practice
The Developmental Argument: Mood Takes Time to Declare Itself
More than half of all mental disorders in adulthood begin in childhood or adolescence [2]. This statistic reveals a crucial clinical reality: early symptoms often predict later struggles, yet the specific disorder may not be apparent initially.
Children showing subthreshold symptoms face increased risk for mental health impairment in adulthood [2]. High-risk youth with family history typically develop major depressive disorder during adolescence, but early warning signs appear much sooner [11]. Anxiety and sleep disturbances in young children increase subsequent mood disorder risk up to 2.5-fold. Even more telling, reduced positive affect rather than excessive negative affect may signal vulnerability to future depression in at-risk children [37].
F39 respects this developmental timeline. The code acknowledges current distress without demanding diagnostic precision that developing brains cannot provide.
The Treatment Argument: Suffering Demands Immediate Response
Four out of five children with diagnosable psychiatric disorders never receive treatment [13]. This gap proves devastating when you consider that subthreshold presentations still cause significant impairment. Young patients struggle at home, school, and with peers regardless of whether their symptoms meet full diagnostic criteria.
Evidence-based treatment approaches work for mood disorders across the spectrum [37]. Early intervention manages current symptoms, reduces severity, and prevents future episodes. Treatment supports normal development while enhancing quality of life and relationships [37]. F39 provides the diagnostic foundation for psychotherapy, family support, and school accommodations without forcing clinicians to wait for full syndrome development.
Delaying intervention until symptoms worsen abandons children to unnecessary suffering.
The Stigma Argument: Labels Have Lifelong Consequences
Mental health stigma remains pervasive. Fifty-one percent of Americans believe people with mental illness face substantial discrimination [3]. Parents reflect this bias—up to 30% report they wouldn't want their child befriending a peer with ADHD or depression [13].
Generation Z shows particular sensitivity to judgment around mental health services, with 49% worrying about disclosure [3]. Stigma prevents teens from accessing help and creates shame when they do seek treatment [3]. Ninety percent of adolescents taking psychiatric medication hide this fact due to stigma [3]. Psychiatric diagnosis can trigger grief and despair, especially when associated with poor outcomes, as some patients struggle to integrate diagnosis with their previous self-image [15].
F39 acknowledges clinical reality without activating the intense stigma attached to specific diagnostic labels.
The Longitudinal Argument: Early Labeling May Be Inaccurate
Childhood internalizing problems lead to varied outcomes in young adulthood, affecting mental health, life satisfaction, educational attainment, and relationships [2]. First-time diagnoses in adolescence show high instability, particularly for affective disorders [47].
Diagnostic bias compounds this uncertainty. Black male teenagers receive schizophrenia diagnoses at significantly higher rates compared to other groups, while white adolescents more readily receive depression diagnoses [16]. Studies show Black adults are diagnosed with psychotic disorders at much higher rates than white adults, even when presenting clear signs of severe depression [16].
Early diagnostic specificity creates momentum. Initial labels persist in medical records despite evolving clinical pictures.
The Identity Argument: Protecting the Developing Self
Adolescence centers on identity formation [4]. Identity diffusion—characterized by fragmented self-concept—underlies severe personality pathology [4]. Psychiatric diagnosis profoundly shapes self-concept during childhood and adolescence, critical periods for identity development [15].
Young people remain particularly sensitive to social influences on identity formation [15]. Illness identity—the degree to which individuals integrate health conditions into their self-concept—significantly affects psychological well-being and social functioning in adolescents with chronic conditions [17].
F39 permits diagnostic humility. The code acknowledges current struggles without foreclosing future possibilities or forcing integration of potentially inaccurate psychiatric identity into the developing self.
The Risks of Premature Diagnostic Specificity
The Borderline Personality Disorder Analogy in Adolescents
Borderline personality disorder affects 1-3% of adolescents and young adults, with onset typically during adolescence even though diagnosis usually doesn't occur before age 18 [6]. This timing gap reveals an important clinical reality: labeling personality pathology during active identity formation carries consequences that extend far beyond simple naming.
Clinicians approach borderline personality disorder diagnosis in young people with notable caution. The reluctance stems from legitimate concerns about diagnosing personality disorders during periods of major developmental change, particularly when the diagnosis includes behaviors that characterize normal adolescence itself [5]. Healthcare professionals often conceptualize these presentations differently or avoid formal diagnosis altogether. Some clinicians deliberately use axis I diagnoses rather than borderline personality disorder due to concerns about how patients will live with that particular label [5].
This diagnostic avoidance creates its own complications. Young people with borderline personality disorder frequently present with multiple comorbidities, leading clinicians to focus assessment and treatment on axis I disorders while core pathology remains unaddressed [5]. Without coordination and involvement of other systems around the young person, intervention effectiveness suffers [5]. Treatment planning becomes unnecessarily complex when the actual diagnosis stays unspoken.
The Pediatric Bipolar Controversy
The pediatric bipolar diagnostic landscape demonstrates how premature specificity generates both overdiagnosis and treatment complications. Between 1994-1995 and 2002-2003, office visits in which children received bipolar diagnoses increased forty-fold, from 25 per 100,000 to 1,003 per 100,000 [9]. This dramatic surge followed efforts to adapt DSM criteria for children by modifying episodicity requirements and accepting chronic irritability as equivalent to manic mood states.
Diagnostic rates in the United States far exceed those in other countries. While 6-19% of children and adolescents in US clinical populations receive bipolar diagnoses, the rate in England is 1.7 cases per 100,000 per year and in Ireland 2.2 cases per 100,000 per year [9]. Countries including Spain, India, Finland, Denmark, and Germany report significantly lower diagnostic rates, with only Brazil approaching the low end of US estimates at 7.2% [9].
Medications used to treat bipolar disorder carry substantial risks. Mood stabilizers and antipsychotics can produce significant side effects, with particular concerns about their effects on developing nervous systems [9]. Children receiving these agents based on loosely applied diagnostic criteria face potential treatment complications if the actual disorder differs from the assigned label.
Antidepressant Risks in Uncertain Diagnoses
Treatment-emergent mania presents a specific concern when antidepressants are prescribed for unipolar depression in youth who may have undiagnosed bipolar spectrum conditions. A large Swedish cohort study of 43,677 children and adolescents aged 4-17 years found that at 12-week follow-up, antidepressant-treated youth showed cumulative mania occurrence of 0.26% compared to 0.20% in untreated controls [8]. Rates rose to 0.79% versus 0.52% by 52 weeks [8].
Risk factors for treatment-emergent mania proved more significant than treatment status itself. Youth on antiepileptics showed a 7.01-fold increased risk, those on antipsychotics a 4.42-fold risk, those with a parent with bipolar disorder a 4.09-fold risk, and those diagnosed with depression in an inpatient facility a 2.27-fold risk [8]. Antidepressant treatment itself was not associated with mania when accounting for these baseline characteristics [8].
The FDA black box warning on antidepressants and suicidality further complicates treatment decisions. Analysis of nearly 400 clinical trials found that 4% of youth under 18 taking antidepressants experienced suicidal behavior or thoughts compared with 2% in placebo groups [18]. No adolescents in the trials died by suicide, yet the warning led to a 30% drop in antidepressant prescriptions after 2004 [18]. Suicide rates in teens and young adults jumped dramatically in the following decade, reversing previous downward trends [18].
Working with Families: Explaining F39 to Parents
Addressing Parental Fears About Unspecified Diagnoses
Parents enter evaluations with heavy concerns weighing on their minds. Is my child normal? Am I to blame? What is the diagnosis? Does my child need treatment? [19]. An unspecified diagnosis often amplifies these worries. Some parents hear "unspecified" as dismissive, as though you haven't taken their child's pain seriously. Others imagine something more serious hiding beneath your reluctance to name it directly.
Every parent brings their own history to these conversations. Their understanding gets shaped by developmental experiences, family patterns, and personal struggles [1]. When parent and child stories don't align, or when concerns vary dramatically, validate their worry while highlighting how complete assessment improves outcomes [1]. Many parents in clinical settings struggle with their own depression and anxiety symptoms. Screening mothers and fathers during child evaluations reveals parental symptoms that can interfere with treatment progress [20].
Your established relationships with families provide significant advantages. These therapeutic connections support social-emotional health at every contact and enable swift intervention when warning signs appear [21]. Children with chronic conditions face higher prevalence of mental health problems than their peers, making these ongoing relationships even more valuable [21].
Sample Language for Clinical Conversations
Focus conversations on observable realities rather than diagnostic uncertainties. "Your child is struggling right now. The irritability, withdrawal, and sleep changes you've described are real symptoms that need our attention. Children's brains continue developing through adolescence, so the exact picture isn't always immediately clear. This diagnosis allows us to start helping your child today while monitoring how symptoms evolve."
Recognize parents as experts on their own child. "You know your child better than anyone. The changes you've noticed are significant enough to bring you here, and that tells me we need to take action." Gather detailed accounts from both parents and child, since parents typically observe behavioral changes while children report internal experiences [1]. Parents notice externalizing symptoms more readily, while children and adolescents identify internalizing symptoms [1].
The Working Diagnosis Frame
Present F39 as a snapshot of current observations rather than a permanent label. "This diagnosis describes what we're seeing today. It gives us the framework to help your child while acknowledging that young people's symptoms can change as they grow and develop." This approach validates family concerns while establishing the foundation for immediate support.
Children find change difficult to process [1]. Shifts in school settings, friend groups, family dynamics, or parental availability often connect to symptom onset. Ask parents directly: "What changes do you think might have triggered these difficulties? What do you believe has contributed to these behavioral shifts?" [1]. Their answers reveal family understanding and identify potential contributing factors.
Psychoeducation About Developmental Trajectories
Explain the developmental perspective clearly. Adolescent cognitive, social, and emotional changes create complex, multifaceted problems that resist simple solutions [1]. Quick advice from clinicians rarely helps unless underlying issues get addressed [1].
Family psychoeducation combined with skills training helps prevent, delay, or reduce the severity of psychiatric episodes [22]. Key goals include building family knowledge about mood conditions, improving communication patterns, and strengthening coping and problem-solving abilities [23]. True psychoeducation goes beyond information sharing to create interactive learning across multiple sessions where families apply concepts to their specific situation and practice new approaches with professional guidance [24].
Help families understand that separating normal developmental challenges from concerning symptoms takes expertise. Seek professional help when behaviors persist for weeks, cause obvious distress, or interfere with school, home, or peer relationships [25].
Clinical Scenarios Where F39 Fits Best
Scenario 1: The Irritable Adolescent Without Clear Mania
A 15-year-old male arrives with three months of daily irritability and angry outbursts. His parents describe oppositional behavior toward teachers and coaches, plus difficulty falling asleep most nights. Irritability accounts for more than 40% of pediatric psychiatric evaluations [26], yet determining the underlying cause remains challenging.
This patient shows persistent baseline irritability rather than distinct episodes [27]. His grandmother has bipolar disorder, raising questions about genetic risk. However, he denies euphoria, grandiosity, decreased sleep needs, or hyperfocused activities. The clinical picture suggests mood dysregulation that doesn't fit bipolar disorder, major depression, or disruptive mood dysregulation disorder criteria.
F39 acknowledges the mood component while allowing time for diagnostic clarity.
Scenario 2: The Somatic Child with Mood Symptoms
An 11-year-old girl presents with four months of recurring headaches, stomach pain, and fatigue. School attendance has dropped significantly. Comprehensive medical evaluation shows no physical causes. Up to 25% of children and adolescents experience chronic somatic pain [28], with these children facing three times higher risk for psychiatric conditions [29].
She reports low mood, lost interest in favorite activities, and withdrawal from friends. Yet symptoms don't meet duration or severity thresholds for major depression. Research shows up to 50% of children with somatic complaints also have psychiatric symptoms [29].
F39 recognizes the mood aspects while avoiding premature depression labeling when physical symptoms dominate the presentation.
Scenario 3: The Post-Traumatic Presentation
A 13-year-old girl presents six weeks after her parents' separation. She shows emotional instability, nightmares, angry episodes, and declining grades. She describes ongoing sadness alongside hypervigilance and concentration problems.
Most children adapt to stressful events without long-term symptoms [7]. PTSD diagnosis requires symptoms persisting beyond one month [7], which hasn't been reached yet. The presentation mixes trauma responses with mood symptoms. Since irritability appears in PTSD criteria across all ages [26], separating trauma effects from primary mood disorders becomes complex.
F39 captures the mood disturbance while preserving time to determine whether symptoms represent emerging PTSD, adjustment struggles, or mood disorder.
Scenario 4: The Emerging Bipolar Spectrum Case
A 16-year-old shows episodes of mood instability and periods of decreased sleep (five hours nightly for several days) without daytime impairment. He demonstrates increased energy for art projects alternating with low motivation phases. Distinguishing bipolar symptoms from normal adolescent mood variations proves difficult [30] [10]. The key indicator remains severe mood swings that differ from typical patterns [10].
His symptoms suggest subsyndromal manic features without meeting full hypomanic episode criteria. Family history includes a mother with bipolar I disorder.
F39 allows mood stabilization interventions while maintaining diagnostic watchfulness as the clinical picture develops.
F39 Documentation Strategies That Protect and Justify
Key Documentation Elements for Medical Records
F39 remains billable for reimbursement purposes [31], yet insurers scrutinize these claims more closely than specific diagnoses [12]. Your documentation becomes your primary defense against audit challenges and claim denials.
Build your case systematically. Include thorough patient history, explicit description of mood disturbances, and clear ruling out of more specific mood disorder categories [32]. Document the factors contributing to diagnostic uncertainty—complex symptoms, atypical presentation, or insufficient duration [14].
Auditors search for specific elements in your notes. They want detailed symptom documentation, differential diagnosis processes, and explanation why more specific codes proved inapplicable [32]. Outline steps taken to exclude specific diagnoses and identify any underlying conditions obscuring full assessment [32].
Your clinical reasoning must be transparent. Document what you observed, what you ruled out, and why F39 represents the most accurate code available. This approach aligns with documentation standards and reduces audit risks [32].
Sample Documentation Template for F39
Structure your notes to withstand scrutiny. Start with observable symptoms and quantified measures. Follow with medical rule-outs, functional impairment documentation, and diagnostic reasoning.
Example documentation: "Patient demonstrates irritable mood with sleep disturbance for 3 weeks. PHQ-A score 14. TSH/CMP within normal limits. Academic performance declined; withdrew from peer activities. Symptom pattern does not meet MDD duration criteria. Atypical presentation (irritability predominant) warrants F39. Plan: weekly psychotherapy, reassess in 6 weeks."
Include your treatment focus and ongoing assessment plan [14]. This transparency protects your clinical decision-making while ensuring appropriate patient care.
Billing and Insurance Considerations
F39 falls within MS-DRG v43.0: 885 Psychoses [31]. The 2026 edition became effective October 1, 2025 [31]. Check individual insurance policies before submitting claims, as some payers impose specific coverage limitations on unspecified mood disorders [12].
Ensure CPT codes align with treatments provided [12]. Regular reassessment proves mandatory [12]. Update records as the clinical picture evolves, transitioning to more specific codes when appropriate [32].
Prepare for potential claim reviews. Document each reassessment point, demonstrating active diagnostic monitoring rather than diagnostic complacency. Be ready to communicate clinical rationale if claims face denial or questioning [12].
Monitoring and Diagnostic Evolution Over Time
F39 Requires Active Reassessment
F39 serves as your starting point, not the final destination [14]. Young patients struggle to articulate their internal experiences, and developmental timelines vary dramatically between children [33]. Regular symptom tracking guides both diagnostic updates and treatment decisions [14].
Research shows patients with unspecified mood disorder diagnoses receive follow-up care for an average of 8.5±10.7 months [34]. The data reveals a clear pattern: longer follow-up periods lead to fewer F39 diagnoses as clinical pictures sharpen [34]. Your role involves actively monitoring this evolution rather than passively waiting for clarity.
Watch for These Diagnostic Red Flags
Certain changes demand immediate diagnostic reconsideration [35]. Clear manic or hypomanic episodes signal bipolar spectrum disorders. Worsening depression that meets full MDD criteria requires diagnostic updating. Psychotic features or suicidal ideation necessitate immediate intervention and diagnostic revision.
Treatment response itself provides diagnostic clues. Poor response to standard interventions may indicate the wrong diagnostic category [14]. Document these observations systematically to support future diagnostic decisions.
Structured Review Every 3-6 Months
Schedule formal reassessments at regular intervals. Review symptom patterns, functional improvements or declines, and treatment effectiveness. New information often emerges during these structured evaluations that warrants diagnostic revision [14].
Making the Transition to Specific Diagnoses
Studies show 25% of patients initially diagnosed with unspecified mood disorder eventually receive depressive disorder diagnoses, while 16.7% transition to bipolar disorder [34]. Make these transitions when symptoms clearly meet full diagnostic criteria for specific conditions.
Document your reasoning thoroughly. Explain the diagnostic change to families and address any concerns about evolving labels [14]. This transparency maintains trust while acknowledging the developmental nature of pediatric mood disorders.
Conclusion
F39 provides clinical honesty in pediatric mood disorder practice. When presentations resist clear categorization, this diagnostic code acknowledges current reality while preserving future possibilities.
Your documentation carries weight. Insurance auditors expect thorough assessment records that justify unspecified coding through comprehensive evaluation rather than incomplete workup. Document your clinical reasoning. Show the steps taken to rule out specific diagnoses. Demonstrate why uncertainty exists despite exhaustive assessment.
Subthreshold presentations demand immediate attention. Children experiencing functional impairment deserve intervention regardless of diagnostic specificity. F39 provides the foundation for treatment initiation while clinical pictures develop.
Monitor actively. Schedule reassessments every three to six months. Watch for emerging patterns that warrant diagnostic transition. Document changes that support moving to specific mood disorder categories when symptoms meet full criteria.
This approach respects the realities of pediatric practice. Developing brains resist premature labeling. Families appreciate diagnostic honesty over forced specificity. Evidence-based treatment can begin immediately while maintaining the clinical humility that pediatric mood disorder work demands.
F39 serves your patients well when used thoughtfully and monitored carefully.
Key Takeaways
Understanding F39 Unspecified Mood Disorder in pediatric practice requires balancing clinical precision with developmental reality, acknowledging that mood symptoms in children evolve as their brains mature.
• F39 requires comprehensive assessment, not incomplete evaluation - Document exhaustive workup, differential diagnosis process, and explicit reasoning for diagnostic uncertainty to justify this billable code.
• Use F39 when mood symptoms cause impairment but resist categorization - Apply when presentations blend depressive/bipolar features, show subthreshold symptoms, or involve somatic complaints with mood components.
• Frame F39 as a "working diagnosis" with families - Explain it acknowledges current suffering while allowing diagnostic clarity to emerge, reducing stigma while enabling immediate treatment.
• Schedule mandatory 3-6 month reassessments for diagnostic evolution - Monitor for red flags like clear manic episodes, worsening depression, or psychotic features that warrant transition to specific diagnoses.
• Premature diagnostic specificity carries risks in developing brains - Early labeling may be inaccurate, trigger stigma, and affect identity formation during critical developmental periods when clinical pictures remain fluid.
F39 serves as a bridge between clinical observation and diagnostic certainty, protecting young patients from premature labeling while ensuring they receive necessary treatment during vulnerable developmental windows.
FAQs
What does the F39 diagnosis mean for my child?
F39 is a diagnostic code for unspecified mood disorder that indicates your child is experiencing mood-related symptoms causing distress or impairment, but the symptoms don't yet fit neatly into a specific category like depression or bipolar disorder. It's a working diagnosis that allows treatment to begin while the clinical picture becomes clearer over time, which is especially important in children whose brains are still developing.
What are the criteria for diagnosing F39 unspecified mood disorder?
F39 is used when a child displays mood disturbances—such as irritability, sadness, or emotional instability—that cause significant problems at school, home, or with friends, but don't meet the full diagnostic criteria for more specific mood disorders. The diagnosis requires comprehensive assessment to rule out other conditions and documentation of why a more specific diagnosis isn't yet appropriate.
How are mood disorders treated in children and adolescents?
Treatment typically includes psychotherapy such as cognitive behavioral therapy (CBT), which helps children understand and manage the connection between their thoughts, feelings, and behaviors. Family involvement, psychoeducation, and sometimes medication may also be part of the treatment plan, depending on symptom severity and the child's specific needs.
Is F39 a permanent diagnosis for my child?
No, F39 is not meant to be permanent. It serves as a starting point that requires regular reassessment every 3-6 months. As your child develops and the symptom pattern becomes clearer, the diagnosis may transition to a more specific mood disorder, or symptoms may resolve with treatment. The unspecified designation reflects current uncertainty, not a lifelong label.
Why would a doctor use an unspecified diagnosis instead of a specific one?
Doctors use F39 when premature labeling could be inaccurate or harmful, particularly in children whose symptoms are still evolving. It allows immediate treatment while avoiding the potential stigma and long-term consequences of a more specific psychiatric diagnosis that may not accurately reflect what emerges as the child matures. This approach balances the need for intervention with diagnostic humility.
References
[1] - https://pmc.ncbi.nlm.nih.gov/articles/PMC9152573/
[2] - https://www.chop.edu/conditions-diseases/mood-disorders-children-and-adolescents
[3] - https://www.cdc.gov/pcd/issues/2024/24_0142.htm
[4] - https://pmc.ncbi.nlm.nih.gov/articles/PMC7856236/
[5] - https://pmc.ncbi.nlm.nih.gov/articles/PMC6022439/
[6] - https://www.merckmanuals.com/professional/pediatrics/psychiatric-disorders-in-children-and-adolescents/somatic-symptom-and-related-disorders-in-children
[7] - https://jamanetwork.com/journals/jamapsychiatry/fullarticle/1937831
[8] - https://pubmed.ncbi.nlm.nih.gov/19465876/
[9] - https://pmc.ncbi.nlm.nih.gov/articles/PMC6393204/
[10] - https://www.psychiatry.org/getmedia/4d6aab2f-87cf-4b22-afc4-8b9035076051/APA-DSM5TR-UnspecifiedMoodDisorder.pdf
[11] - https://therapistdevelopmentcenter.com/blog/dsm-5-tr-reinstating-unspecified-mood-disorder?srsltid=AfmBOorJCR2zA0AaLBDdCPHf_mc8ZdYVlTY6Sj_uaV7ugV9wfBdD3TLc
[12] - https://genhealth.ai/code/icd10cm/F39-unspecified-mood-affective-disorder
[13] - https://www.sprypt.com/behavioral-health-icd-codes/f39
[14] - https://www.blueprint.ai/blog/mood-disorder-icd-10-understanding-code-f39-and-navigating-unspecified-mood-disorders-in-clinical-practice
[15] - https://www.icd10data.com/ICD10CM/Codes/F01-F99/F30-F39/F39-/F39
[16] - https://pmc.ncbi.nlm.nih.gov/articles/PMC8734087/
[17] - https://pmc.ncbi.nlm.nih.gov/articles/PMC11235047/
[18] - https://pmc.ncbi.nlm.nih.gov/articles/PMC3419431/
[19] - https://www.brownhealth.org/be-well/stigma-and-mental-illness
[20] - https://meridianpsychiatricpartners.com/the-dangers-of-mental-health-stigma-to-adolescents/
[21] - https://www.sciencedirect.com/science/article/abs/pii/S0277953618303678
[22] - https://www.researchgate.net/publication/395408226_Diagnostic_trajectories_and_stability_of_mental_disorders_in_childhood_and_adolescence_-_A_nation-wide_cohort_study_using_sequence_analysis
[23] - https://childmind.org/article/misdiagnosis-of-mood-disorders-in-teenagers-of-color/
[24] - https://pmc.ncbi.nlm.nih.gov/articles/PMC3751041/
[25] - https://www.frontiersin.org/journals/public-health/articles/10.3389/fpubh.2025.1713205/full
[26] - https://www.acog.org/clinical/clinical-guidance/committee-opinion/articles/2017/07/mental-health-disorders-in-adolescents
[27] - https://www.ncbi.nlm.nih.gov/books/NBK55399/
[28] - https://pmc.ncbi.nlm.nih.gov/articles/PMC2846895/
[29] - https://www.psychiatryadvisor.com/news/antidepressants-and-risk-for-manic-episodes-in-youth/
[30] - https://news.stanford.edu/stories/2025/07/antidepressants-kids-teens-science-research
[31] - https://www.aacap.org/AACAP/Families_and_Youth/Facts_for_Families/FFF-Guide/Comprehensive-Psychiatric-Evaluation-052.aspx
[32] - https://pmc.ncbi.nlm.nih.gov/articles/PMC6345125/
[33] - https://pmc.ncbi.nlm.nih.gov/articles/PMC3083121/
[34] - https://publications.aap.org/pediatrics/article/144/5/e20192757/38256/Mental-Health-Competencies-for-Pediatric-Practice
[35] - https://pmc.ncbi.nlm.nih.gov/articles/PMC10503895/
[36] - https://www.aacap.org/App_Themes/AACAP/Docs/member_resources/family_psych_toolkit/evidence/Clinics_2015-Childhood_Mood_DIsorders.pdf
[37] - https://pmc.ncbi.nlm.nih.gov/articles/PMC7416523/
[38] - https://www.cdc.gov/children-mental-health/about/index.html
[39] - https://psychiatryonline.org/doi/10.1176/appi.ajp.2016.16040429
[40] - https://www.additudemag.com/irritability-dmdd-adhd-odd-bipolar-children/?srsltid=AfmBOoqJJdOHgdzYNNsbz3cK5gytreHQE43drrH1oq4KzCo_o79joDnO
[41] - https://www.cdc.gov/children-mental-health/about/post-traumatic-stress-disorder-in-children.html
[42] - https://www.nimh.nih.gov/health/publications/bipolar-disorder-in-children-and-teens
[43] - https://www.mayoclinic.org/diseases-conditions/bipolar-disorder/symptoms-causes/syc-20355955
[44] - https://www.simplepractice.com/icd-10-codes/f30-f39/f39/
[45] - https://www.mayoclinic.org/healthy-lifestyle/childrens-health/in-depth/mental-illness-in-children/art-20046577
[46] - https://dusunenadamdergisi.org/article/82/pdf
[47] - https://www.kennedykrieger.org/stories/making-difference/inspiring-stories/red-flags-mental-health-what-parents-should-know
If you’re ready to spend less time on documentation and more on therapy, get started with a free trial today
Not medical advice. For informational use only.
Outline
More articles