VR and Depression: What The 'Darkening' Exhibition Reveals About Empathy Through Technology

Feb 23, 2026
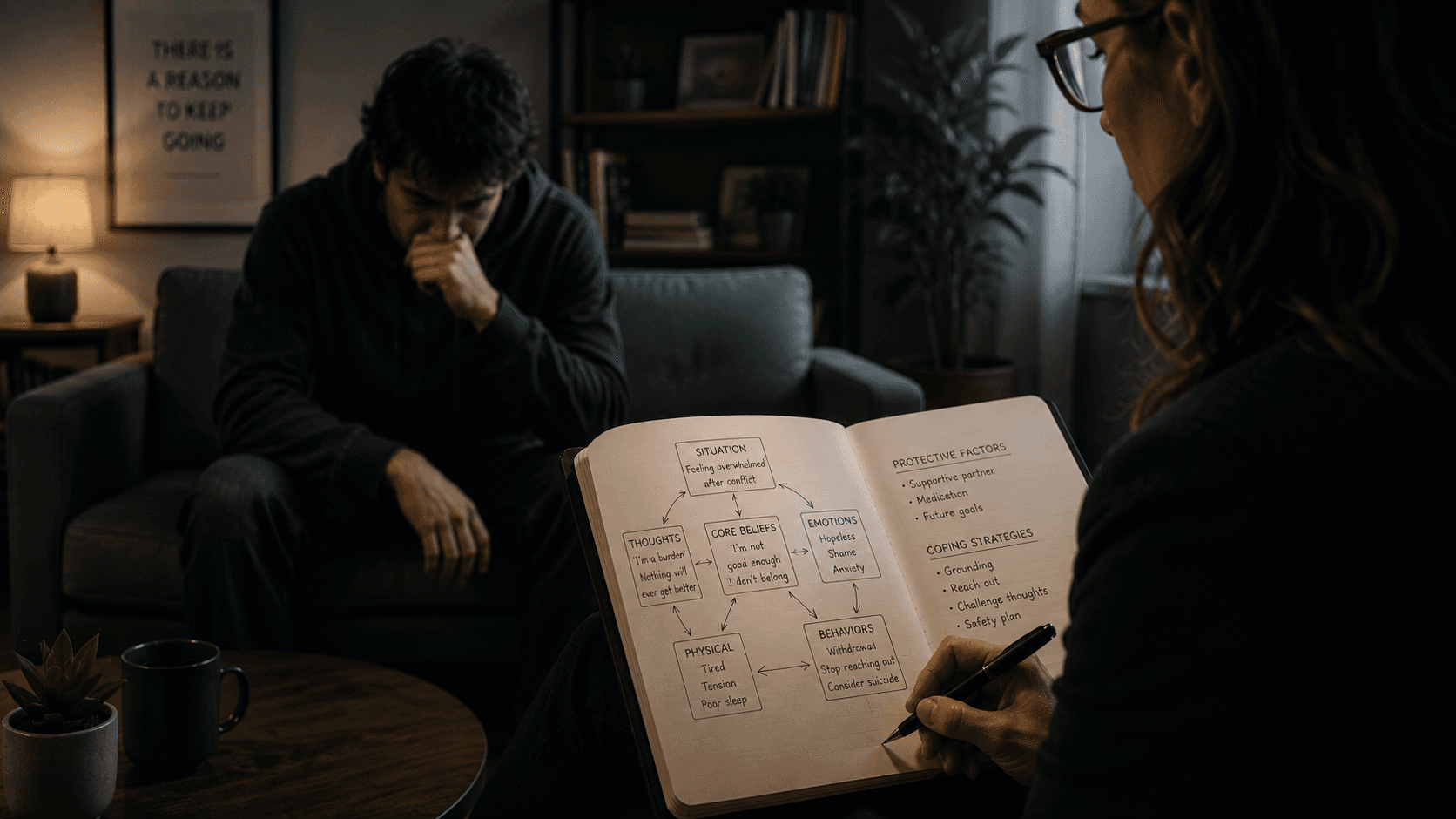
Mental health professionals face a persistent challenge: bridging the gap between observing depression and understanding its lived reality. Clinical assessment tools like the PHQ-9 capture symptoms effectively. They measure sleep disturbance, appetite changes, and concentration difficulties. What they cannot measure is the suffocating weight patients describe, the way colors drain from everyday experiences, or how minutes stretch into hours when depression takes hold.
Ondřej Moravec's 'Darkening' offers a different approach. This 18-minute VR experience guides viewers through his personal journey with depression, creating an immersive window into the condition's subjective landscape [52]. Rather than reading case studies or reviewing symptom checklists, mental health professionals can step inside the phenomenological world their patients inhabit.
The evidence supports VR's potential for clinical education. Research demonstrates that 97.5% of participants in VR mental health programs reported positive impacts on their understanding [52]. These programs consistently show improved attitudes and reduced stigma following VR psychoeducation interventions [52]. For a field built on empathy and connection, VR empathy training represents a practical tool for deepening therapeutic relationships and clinical insight.
The Phenomenology of Depression: What Words Cannot Capture
The Ineffable Core of Depression
Depression creates a cruel paradox. The very condition that patients need to describe disrupts their ability to articulate the experience [52]. Mental disorders influence how people access and describe their own experiences, creating what researchers call a fundamental methodological challenge: the condition impairs the ability to explain that understanding.
This goes beyond clinical inconvenience. It raises questions about the reliability of patient descriptions themselves.
Philosopher Matthew Ratcliffe offers a framework for understanding this challenge. Depression operates not as an intentional state but as an alteration in "existential feeling"—our pre-conscious, embodied sense of belonging to a shared world [52]. This existential feeling shapes how we experience being alive, distant, detached, or overwhelmed before we develop words for these states [52]. Patients often say "things just don't feel right" or "I feel out of it," gesturing toward something language cannot fully capture [52].
The silence can become complete. Some patients lose speech entirely during severe episodes, as one writer described: a time "when my depression was so heavy my tongue wouldn't move" [52]. This double silence—internal and external—traps individuals without knowing when escape might come [52]. The loss extends beyond words to social agency itself, with one patient describing attempts "to utter small talk, and be responsive to questions" as "a fierce trial" [52].
The Limits of Clinical Scales
Every assessment tool faces built-in constraints. The PHQ-9 remains one of the most widely used depression scales globally, yet patients consistently report it fails to reflect their actual experiences [52]. Study participants felt unable to engage with PHQ-9 items meaningfully, producing inaccurate answers and mismatched results [52]. They found the scale too crude, offering no way to express the true extent of their symptoms [52].
Each scale carries specific limitations:
HAMD: Requires professional assessors, adding complexity [27]
BDI: Offers comprehensive dimensions but includes difficult-to-understand items [27]
CES-D: Struggles with unclear differentiation between emotional and somatic symptoms [27]
PHQ: Works for rapid screening but lacks sufficient emotional evaluation [27]
These tools capture symptom presence, not symptom experience. Anhedonia becomes a checked box rather than the lived absence of pleasure. Sleep disturbance gets quantified without conveying the texture of lying awake in darkness. Patient descriptions themselves may become over-generalized and pessimistic, reflecting the same negative stories they view as permanent and pervasive [52]. Essential experiential details remain hidden [52].
The Empathy Challenge for Clinicians
Ratcliffe proposes "radical empathy" as the required clinical stance—attentiveness that stays open and curious about how another's experience might differ from our own [52]. Radical empathy means engaging with patient experiences while suspending assumptions that both parties share the same possibilities [52]. This demands acknowledging an experientially constituted reality and committing to study it further [52].
The challenge deepens because empathy operates across multiple dimensions that relate differently to depression. Perspective-taking, which reflects cognitive empathy, predicts depression negatively. Personal distress, reflecting affective empathy, predicts depression positively [52]. Research shows personal distress has the highest positive bridge expected influence in empathy-depression networks [52].
For clinicians, this means different empathic approaches produce different outcomes—some protective, others potentially harmful.
Even skilled therapists rely on analogy and intellectual understanding without direct experience. These approaches remain valuable but incomplete. The gap between observing symptoms and inhabiting the phenomenological world of depression persists, regardless of our clinical expertise and good intentions.
VR as an Empathy Machine
Virtual embodiment shifts the relationship between observer and observed. Head-mounted displays replace a user's visual field with a virtual body, creating experiences far beyond traditional documentaries or case studies. Body-tracking technology enables synchronous virtual movements, generating what researchers call the "illusion of virtual body ownership" where individuals perceive the virtual body as their own, regardless of differences in appearance, age, race, or condition [52].
How VR Creates First-Person Experiences
Five key elements drive VR's impact on empathy: immersion, presence, engagement, illusion of virtual body ownership, and agency [52]. Immersion creates vivid virtual environments while blocking physical reality [52]. Presence generates the sense of "being there" in virtual space [47]. Virtual embodiment allows participants to inhabit another's perspective rather than imagine it.
This literal perspective-taking produces measurably different outcomes than traditional empathy exercises. Studies consistently show immersive VR generates stronger empathic responses than non-immersive formats [52]. Participants who experienced embodied first-person scenarios showed increased helpful behaviors toward outgroup members compared to those who merely imagined another's perspective [52].
The precision matters for clinical applications. VR can simulate different skin tones, ages, genders, or disabilities while maintaining experimental control [47]. Researchers have successfully reduced implicit racial bias, reversed in-group prejudice, and decreased discrimination toward older adults [52]. For mental health, this means individuals without depression can experience simulated symptoms from a first-person perspective, potentially shifting their view of mental illness from outgroup to ingroup [52].
Research Evidence on VR Reducing Stigma
Stanford's Virtual Human Interaction Lab created "Becoming Homeless," a seven-minute experience where participants navigate post-job loss scenarios. Results showed sustained attitude change beyond other media. 82 percent of participants in the VR condition signed a petition supporting affordable housing versus 67 percent who read narratives [52]. A second study found 85 percent versus 63 percent [52].
The longitudinal evidence proves particularly compelling. Participants who experienced VR showed significantly greater agreement with statements like "Our society does not do enough to help homeless people" weeks after the intervention [52]. One participant emailed researchers months later about befriending a homeless person in their community [52].
Mental health care staff participated in a study examining VR simulations of psychotic experiences including auditory hallucinations in home scenarios [52]. The VR intervention group scored significantly higher on user satisfaction than controls [52]. Participants described the experience as "immersive" and "realistic," appreciating how it revealed not only psychotic features and negative emotions but their debilitating effects on orientation, state of mind, and overall functioning [52].
The mechanism appears to be experiencing distressing psychopathology firsthand, which generates greater concern for patients and improved attitudes [52].
Studies simulating daily life experiences of people with mixed anxiety and depressive disorder found both immersive VR and text with audio narration successfully reduced public stigma, with effects sustained at one-week follow-up [52]. The approach mattered. This study purposely minimized symptom simulations, instead constructing the everyday living experience of the protagonist as a person rather than a collection of symptoms [52].
Therapeutic Strategies VR Can Target
VR interventions address multiple therapeutic mechanisms:
Psychoeducation
Behavioral activation
Cognitive restructuring
Enhancing positive affect
Mental imagery
Skills training
Cognitive functioning
A Stanford study following 26 people with major depressive disorder found VR headsets for behavioral activation showed similar efficacy to traditional real-world behavioral activation [27].
Healthcare organizations increasingly adopt VR interventions to enhance training quality, including mental health care [52]. The immersive nature creates scenarios users experience more realistically than traditional videos [52]. Sense of embodiment and story transportation associate sequentially with public stigma reduction [52], suggesting the pathway operates through both cognitive identification and emotional immersion.
First-person anti-stigma VR interventions outperform video interventions, benefiting from increased presence and embodiment toward patients with depression [47]. Enhanced presence and embodiment, achieved through immersive storytelling and first-person perspective avatar interactions showing recovery, influence empathy and knowledge retention [47].
Case Study: 'Darkening' — Ondřej Moravec's VR Journey
The Artist and His Vision
Moravec discovered VR through his work as program director for One World festival in Prague, where he programmed the festival's first VR selections in 2014 [52]. The medium's focus on personal experiences caught his attention. He began questioning which topic felt close enough to warrant his own exploration [52]. Depression emerged as the natural choice—people consistently asked him what living with the condition actually felt like [52].
The decision to create something explicitly about himself required courage. Moravec chose to use himself as what he called a "guinea pig" [52]. His journalism background at Czech Television provided the foundation. Every project he creates stays rooted in reality [52].
Frame Films producer Hana Blaha Šilarová joined the production alongside co-producers NowHere Media from Germany and Brainz Immersive from Czech Republic. Bára Anna Stejskalová created the artwork [54]. Czech Film Fund supported the project, making it the first Czech VR film to receive such backing and premiere at an A-list festival [55]. Venice Immersive 2022 selected 'Darkening,' leaving Moravec watching "with your mouth open" as his dream became reality [55].
What Viewers Experience in 'Darkening'
The experience follows Moravec from childhood through his professional years. Viewers inhabit his perspective during first depressive episodes on a family trip, at university while pursuing perfect results, and later at work facing what he calls the depressive "darkening" [56]. Sessions last between 18 and 25 minutes depending on the version [57] [54].
Stylized animation represents Moravec's environment while abstract imagery conveys his emotions [56]. This visual approach allows viewers to witness symptoms gradually taking shape across different life stages [58]. The story moves through diverse landscapes that mirror his struggle with depression since puberty [56].
Voice control sets 'Darkening' apart from other VR experiences [55]. This design choice reflects Moravec's personal discovery that voice became his primary tool for managing depression [56]. Humming, singing, and shouting serve as his calming and relieving techniques [56]. The film makes this therapeutic approach interactive—visitors use VR headsets individually and can respond vocally, though participation remains optional [58]. This active engagement deepens emotional connection and honors the quiet, daily efforts people make to manage their mental health [58].
Co-producer and technology partner Robin Pultera explained that voice control allows viewers "to feel the experience more strongly as if they were part of the story itself" [55]. The interactive design enables viewers to literally touch Moravec's world and offer the protagonist support [55].
The Curatorial Intent Behind the Exhibition
Moravec aimed to spark conversation about what he terms "pains of the soul" [55]. Exhibition venues like DOX in Prague and the National Center for Mental Health in Seoul featured four VR stations, accommodating four viewers per session [53] [57]. This group format created what observers described as "disassociated sort of social dynamics" as participants could overhear others experiencing moments of catharsis [53].
Venice Immersive presentations included Moravec leading post-screening discussions, creating space for viewers to reflect and share similar experiences [53]. He found this facilitation challenging, balancing preparation for intimate questions while maintaining appropriate boundaries around personal disclosure [53].
The Korean-dubbed version, developed with Czech Center Seoul, enabled deeper audience engagement [57]. Educational programs brought the film to high schools, where Moravec met teachers ranging from highly engaged with mental health topics to others needing guidance about depression's debilitating effects [52]. Students regularly approached him after screenings, expressing gratitude for helping them identify with someone facing similar struggles [52].
What Clinicians Can Learn from 'Darkening'
The Texture of Anhedonia
Clinical scales identify anhedonia as reduced interest or pleasure. 'Darkening' reveals the lived absence behind that clinical description. Approximately 70% of patients with major depression show clinically significant anhedonia [6], yet the texture of this absence remains difficult to convey. Recent research distinguishes between wanting, liking, and learning components of pleasure [12]. Patients might retain the ability to judge duration accurately while subjectively experiencing time as crawling [13].
VR art therapy depression experiences allow viewers to inhabit environments where nothing stands out, where effort yields no reward. Research shows anhedonia associates with severe social dysfunction, higher rates of withdrawal, and impaired ability to anticipate pleasure even when actual experience remains intact [6]. Depression creates deficits in appraisal rather than sensory pleasure itself [14]. Viewers report feeling the weight required to engage with a world offering nothing back.
The Experience of Slowed Time
Major depression subjectively removes the ability to influence the present, creating an impersonal and blocked future where time becomes dragging, inexorable, viscous [15]. Meta-analysis across 16 studies found medium effects of depression on time perception, with depressed individuals consistently reporting time passing extremely slowly or standing still [16] [17]. Their estimates of actual time intervals remained as accurate as healthy controls [13].
The present renders itself meaningless, the past unchangeably negative [15]. One patient described: "Time seemed an eternity" [2]. VR simulates this temporal dilation in ways verbal description cannot, allowing clinicians to experience how moments stretch while the future collapses.
The Internal Critic Made Visible
Self-criticism plays a pivotal role in psychological distress and links to poor treatment outcomes [18]. The roots trace to childhood, where children internalize external views, predominantly parental criticism [19]. Chairwork interventions addressing self-criticism show notable reductions in depressive symptoms with large effect sizes [18].
Patients describe relentless destructive chatter. VR mental health education experiences externalize this as shadow figures or voices. Viewers encounter what it feels like to have a constant, undermining presence. One patient reported: "The thoughts just come... I try to stop them, but I can't" [2].
The Fragility of Relief
Treatment-resistant depression affects many individuals despite antidepressants and psychotherapy [20]. Anhedonia persists as a residual symptom, contributing to reduced therapy compliance and increased relapse risk [6]. Meditation shows 10% to 20% improvement in depression symptoms [21], yet the ground for hope itself erodes [2].
Moments of color, lightness, or connection appear then vanish in artistic representations. Viewers experience the instability of positive affect and sense that relief remains temporary, contingent. Participants reported normalization of time experience while engaged in social activities, but symptoms returned [15].
The Isolation That Depression Creates
Depression functions as "an illness of isolation, a disease of disconnection" [7]. The ability to enter we-experiences erodes due to overwhelming feelings of being different and misunderstood [7]. Individuals retain the capacity to understand others, but connection profoundly alters [7]. The peculiarly painful mark lies in desiring connection while feeling robbed of the ability to achieve it [7].
VR clinical supervision tools paradoxically simulate this through solitary headset experiences. You remain alone inside an experience others cannot access, mirroring how depression isolates even in crowded rooms. One patient described: "I feel completely cut off from the rest of humanity... I am a walking corpse" [2].
VR in Clinical Education and Supervision
Current Applications in Medical Education
Medical schools are adopting VR empathy training as a standard component of clinical education. Virtual and augmented reality create standardized, repeatable learning experiences that traditional methods cannot match [22]. Psychiatric education benefits particularly from VR simulations, giving students access to clinical scenarios rarely available during limited placement rotations [22]. Students consistently report high satisfaction with VR experiences, especially when simulations offer realistic detail and meaningful interaction [22].
Mental health nursing programs show concrete educational outcomes. VR simulation systems use multiple sensors to visualize and replicate psychotic symptoms, allowing students to experience what patients encounter [23]. Nursing students report that 360° VR simulations depicting real patients with psychiatric symptoms significantly improve their clinical understanding [23]. The technology bridges a critical gap, providing students without direct clinical experience realistic patient encounters and deeper understanding of mental health conditions [23].
Occupational therapy students at Oxford Brookes University practice conversations with patients experiencing suicidal ideation through VR, then switch perspectives to experience the interaction from the patient's viewpoint. Students report feeling better prepared and more empathetically aware following these role-reversal exercises.
Social Work Training Programs Using VR
The University of Kentucky College of Social Work created VR simulations specifically for child welfare investigations [1]. Students conduct virtual home visits, perform interactive interviews, and assess risks and symptoms of child maltreatment in controlled environments [24]. These simulations, based on actual cases of abuse and neglect, allow students to practice the complete range of investigative skills before encountering real families [1].
Dean Jay Miller emphasizes the necessity: "It's really difficult to capture the true essence of what it's like to go out and investigate an incidence of child maltreatment. This allows for a depth of experience that you can't mimic in any other space" [1]. Students learn de-escalation techniques in situations where virtual clients become angry, building crucial skills in a safe environment [1].
Miami University social work students engage with five VR modules covering elder abuse and neglect scenarios [25]. The immersive case studies reveal unfiltered interactions, family cultural dynamics, living conditions, and medical appointment realities [25]. Faculty observe that students develop both genuine empathy for clients and practical understanding of social work roles through these realistic scenarios [25].
Applications for Experienced Clinicians
VR offers experienced therapists something beyond basic skill development: access to renewed phenomenological understanding. Seasoned clinicians benefit from fresh contact with the subjective experiences their patients navigate daily. Artistic VR experiences like 'Darkening' serve different purposes than clinical training modules, providing interpretive space and emotional ambiguity rather than standardized learning outcomes.
Using VR in Supervision Groups
The pandemic accelerated online group therapy adoption, but two-dimensional screen interactions limit important human connection elements [26]. Lack of genuine eye contact, turn-taking difficulties, and heightened self-consciousness create barriers to meaningful group engagement [26]. Virtual reality addresses these limitations as affordable, high-quality headsets become more accessible to clinical practices [26].
VR support groups create shared 360-degree digital environments where participants can connect meaningfully [5]. This mutual immersion enables intimate interactions impossible through video or phone platforms [5]. Each participant creates their own avatar, providing anonymity that helps people overcome hesitation and share personal experiences more openly [5].
Supervision groups viewing identical VR experiences develop shared reference points for deeper clinical discussions: "When the colors briefly returned, I felt hope—then devastation when they faded. Is that what our patient means when she says she can't hold onto good moments?"
Using VR in Clinical Dialog with Patients
Creating Shared Reference Points
Stanford researchers followed 26 adults diagnosed with major depressive disorder through a four-week behavioral activation trial [27]. Participants met weekly with a clinical psychologist who assigned homework between sessions: scheduling at least four pleasurable activities each week, either in virtual reality or real life [27]. After four weeks, both groups saw significant decreases in their symptoms of depression on widely used scales [27].
The most revealing finding came from participant feedback. Using VR inspired people to get out and do things in the real world [27]. These virtual activities got their motors running just enough to get out of bed [27]. VR became a bridge, not a destination.
This creates new conversational pathways for clinicians. When patients struggle to articulate their experience, VR provides shared reference points. Questions shift from abstract ("How are you feeling?") to specific ("What from that experience felt familiar to you?"). The shared language accelerates understanding and builds stronger therapeutic connections.
Patient Validation Through Immersive Experience
Psychoeducation through VR invites individuals to step into scenarios and address their concerns in reality-adjacent ways [10]. The interactive nature triggers the senses and involves body movement, evoking greater connection to the experience [10]. Learning about mental health becomes an immersive process rather than passive information transfer [10].
Patients often report profound validation when clinicians demonstrate understanding of the experience of depression, not just its symptoms. VR accelerates this validation by allowing clinicians to inhabit, momentarily, the phenomenological space patients describe.
Self-compassion interventions using virtual avatars show promise. Individuals engaged with avatars, offering both criticism and compassion to themselves [10]. As self-compassion increased, self-criticism decreased, reducing depression risk [10]. Externalizing criticism through an avatar helped individuals address these thoughts effectively [10].
Family Understanding Through VR
Family psychoeducation (FPE) focuses on illness as the object of treatment, not the family itself [28]. Meta-analysis of five studies with 301 patients with MDD and their family members showed statistically significant improvement in patients' symptoms at 16 weeks and at final follow-up [28]. FPE consisted of sessions where caregivers learned about depression and implemented appropriate coping strategies [28].
Virtual social skills training has proven effective for individuals with autism and schizophrenia, a foundation that holds promise for depression treatment [10]. For families struggling to understand why a loved one "can't just cheer up," VR experiences provide visceral comprehension that conversations alone cannot achieve.
Safety Considerations and Limitations
Despite evidence supporting VR effectiveness, adoption in therapy remains low [4]. Barriers include lack of knowledge and training, financial constraints, and concerns about the therapeutic relationship [4]. Some participants expressed that VR conflicts with specific therapeutic approaches, fearing it could be a barrier for patients [4].
VR can cause cybersickness: nausea, disorientation, headaches, dizziness, fatigue, sweating, and eye strain [11]. Its immersive nature can be retraumatizing or exacerbate fear, paranoia, or psychosis [11]. Individual characteristics including age, personality, and history of motion sickness must be considered [29]. VR serves as a complementary tool, not a substitute for usual methods [29].
Ready to explore how advanced technology can enhance your clinical practice? Yung Sidekick offers AI-powered session analysis and progress notes that help you stay fully present with your clients while capturing every important detail. Our secure, HIPAA-compliant platform integrates seamlessly with your existing workflow, allowing you to focus more on therapeutic relationships and less on administrative tasks.
The Evidence Base: What We Know and Don't Know
What Research Shows About VR and Empathy
Current research supports VR applications across multiple mental health conditions. A systematic review of 721 studies demonstrates benefits for anxiety disorders, autism spectrum disorder, PTSD, dementia, schizophrenia spectrum disorders, and addiction [30]. VR exposure therapy for anxiety and trauma-related disorders shows the strongest evidence base, with numerous meta-analyses confirming efficacy [30].
Empathy research reveals more mixed findings. Medical students showed significant correlations between immersion aspects and empathy scores (r = .308, P = .049) and presence aspects (r = .415, P = .01) [31]. However, single VR experiences proved insufficient to produce significant empathy improvements [31]. Studies comparing VR to 2D video for schizophrenia stigma found both methods effective, though VR showed greater impact on attitude and knowledge change [9].
Questions That Remain Unclear
The evidence base contains significant gaps. Villalba's review of 2015-2020 literature found insufficient rigorous, empirical scientific evidence proving VR definitively develops empathy [3]. Sora-Domenjó's review revealed limited empirical evidence linking VR exposure to increased empathy that motivates prosocial behavior [3].
Quality concerns persist across studies. A meta-analysis found immersive VR generally effective for mental health disorders, yet approximately half the reviewed studies carried high risk of bias due to inadequate information on randomization and assessor blinding [32]. Evidence certainty was judged as low to very low [32]. Most studies used small sample sizes, limiting statistical power [32].
Artistic VR vs Clinical VR Tools
'Darkening' represents artistic expression rather than clinical intervention. For mental health professionals, artistic VR may offer unique value precisely because it provides what clinical tools often lack: ambiguity, metaphor, and space for personal interpretation.
Clinical VR tools focus on measurable outcomes and standardized experiences. Artistic VR experiences like 'Darkening' create emotional resonance and phenomenological understanding that may prove equally valuable for clinical education and supervision.
Future Research Directions
Establishing VR's role in mental health education requires larger-scale studies, standardized protocols, and structured clinician training programs [30]. Research must address efficacy, tolerability, and implementation barriers before broader adoption [32].
Priority areas include developing best practices for different clinical populations, understanding long-term effects of VR empathy training, and creating guidelines for ethical application in therapeutic settings.
Practical Considerations for Clinicians
How to Access VR Experiences Like 'Darkening'
'Darkening' and similar works appear at film festivals, art exhibitions, and increasingly on VR platforms accessible through Meta Quest or Apple Vision Pro headsets [33]. Professional organizations now offer VR experiences as part of continuing education programs.
The adoption gap remains significant. Only 7.1% of clinicians currently use VR in practice [8]. However, 42.3% indicated plans to adopt it after watching a short informational video [8]. This suggests that educational exposure proves key to supporting VR integration into clinical practice [8].
Start small. A brief introduction to VR capabilities can shift perspectives dramatically.
Integrating VR into Your Practice
Begin with personal exploration before recommending VR to patients or using it in supervision sessions. View experiences with colleagues and discuss what each person noticed. Different perspectives often reveal insights you might miss alone.
VR references can open dialog with patients who struggle to articulate their experience or show interest in technology. Family psychoeducation using VR might help relatives understand depression more deeply, given that traditional family psychoeducation shows statistically significant improvement in depression symptoms at 16 weeks [33].
Consider your practice's specific needs. Some therapists find VR most valuable for training purposes. Others use it to create shared reference points with patients who have difficulty describing their internal experience.
Ethical Considerations and Boundaries
VR experiences can be intense. Some individuals find mental health simulations triggering [34]. Never require patients or families to view potentially distressing content.
Screen for contraindications before recommending VR experiences:
Seizure disorders
Severe vestibular issues
Active psychosis or dissociation [35]
Physical side effects including simulator sickness affect some users [30]. Watch for signs of discomfort during or after VR sessions.
Maintain clear clinical boundaries. VR serves as a complementary tool, not a substitute for established therapeutic methods [29]. Your clinical judgment remains the primary guide for patient care.
Conclusion
Technology critics worry about digital tools creating distance between people. VR applications in mental health education suggest the opposite may be true. When used thoughtfully, immersive technology can deepen our understanding of experiences that remain difficult to communicate through traditional methods.
Depression creates a subjective reality of weight, muted colors, and distorted time perception. Clinical scales capture symptoms effectively but cannot convey this lived experience. VR experiences like 'Darkening' provide mental health professionals with direct access to these phenomenological states, creating shared reference points that enhance therapeutic dialogue.
The clinician who experiences 18 minutes of Moravec's journey may approach patient conversations differently. Instead of relying solely on symptom checklists, they carry experiential knowledge that informs their listening. This shift from observing depression to momentarily inhabiting its landscape represents a meaningful advancement in clinical empathy and understanding.
Mental health practice continues to benefit from tools that strengthen the therapeutic relationship. VR technology, when applied with appropriate clinical boundaries and ethical considerations, offers one such tool. As adoption increases and research evidence grows, these immersive experiences may become valuable components of clinical education and supervision.
Disclaimer: This article explores emerging technologies for clinical education and does not constitute medical advice or treatment recommendations.
Key Takeaways
VR technology is revolutionizing how mental health professionals understand and treat depression by creating immersive, first-person experiences that traditional clinical tools cannot provide.
• VR creates empathy through embodiment: Unlike reading case studies, VR allows clinicians to literally inhabit a patient's perspective, with 97.5% of participants reporting positive impacts on understanding mental health conditions.
• Traditional depression scales miss the lived experience: Tools like PHQ-9 measure symptoms but cannot convey the weight, grayness, and slowed time that patients describe as central to their depression.
• 'Darkening' demonstrates VR's clinical potential: This 18-minute immersive experience by Ondřej Moravec allows viewers to experience depression's phenomenology, creating shared reference points for deeper clinical dialog.
• Evidence shows sustained attitude change: Stanford research found VR empathy training produced lasting behavioral changes, with 85% of participants supporting policy changes weeks after the experience versus 63% in control groups.
• Integration requires careful ethical consideration: While promising, VR can cause cybersickness and may be retraumatizing for some patients, requiring proper screening and positioning as a complementary tool, not replacement for traditional therapy.
VR represents a new frontier in clinical education and patient understanding, offering unprecedented access to the subjective reality of mental illness while requiring thoughtful implementation and ongoing research validation.
FAQs
Q1. How does virtual reality help clinicians better understand depression compared to traditional assessment tools?
Virtual reality creates immersive, first-person experiences that allow clinicians to inhabit the phenomenological world of depression—experiencing the weight, grayness, and slowed time that patients describe. Traditional clinical scales like the PHQ-9 measure symptoms but cannot convey the lived texture of depression. Research shows 97.5% of participants in VR mental health programs reported positive impacts on their understanding, with VR producing deeper empathy than reading case studies or watching videos.
Q2. What is the 'Darkening' VR experience and what does it reveal about depression?
'Darkening' is an 18-minute immersive VR experience created by Ondřej Moravec that guides viewers through his personal journey with depression from childhood through adulthood. Using animation and voice-controlled interaction, it allows viewers to experience anhedonia, temporal dilation, internal criticism, and the isolation that depression creates. The experience premiered at Venice Immersive 2022 and has been used in educational settings to help students, families, and clinicians understand what living with depression truly feels like.
Q3. Can VR experiences actually reduce stigma around mental health conditions?
Yes, research demonstrates that VR experiences produce measurable and sustained reductions in mental health stigma. Stanford studies found that 85% of participants who experienced VR simulations supported policy changes to help affected populations, compared to 63% in control groups. Mental health care staff who participated in VR simulations of psychotic experiences reported significantly higher satisfaction and developed greater concern for patients. The effects persisted weeks after the intervention, with participants showing lasting attitude changes.
Q4. What are the risks and limitations of using VR in mental health treatment?
VR can cause cybersickness including nausea, disorientation, headaches, and eye strain in some users. Its immersive nature may be retraumatizing or exacerbate symptoms for individuals with active psychosis, dissociation, seizure disorders, or severe vestibular issues. Currently, only 7.1% of clinicians use VR in practice, with barriers including lack of training, financial constraints, and concerns about the therapeutic relationship. VR should serve as a complementary tool rather than a replacement for traditional therapeutic methods.
Q5. How can mental health professionals integrate VR into their clinical practice?
Clinicians should start by personally exploring VR experiences before recommending them to patients or using them in supervision. VR can be integrated through continuing education programs, group supervision discussions, family psychoeducation sessions, and as conversation starters with patients who struggle to articulate their experiences. However, proper screening for contraindications is essential, and clinicians should never require patients to view potentially distressing content. Short educational sessions about VR have been shown to increase clinician adoption rates from 7.1% to 42.3%.
References
[1] - https://www.korea.net/Government/Briefing-Room/Press-Releases/view?articleId=1488746&insttCode=A260111&type=N
[2] - https://pmc.ncbi.nlm.nih.gov/articles/PMC11938894/
[3] - https://mental.jmir.org/2025/1/e66925
[4] - https://www.frontiersin.org/journals/psychology/articles/10.3389/fpsyg.2023.1215388/full
[5] - https://ndpr.nd.edu/reviews/experiences-of-depression-a-study-in-phenomenology/
[6] - https://link.springer.com/article/10.1007/s11229-025-04933-8
[7] - https://bmjopen.bmj.com/content/7/4/e014519
[8] - https://pmc.ncbi.nlm.nih.gov/articles/PMC12065149/
[9] - https://www.frontiersin.org/journals/public-health/articles/10.3389/fpubh.2022.1034119/full
[10] - https://www.jmir.org/2021/7/e23683/
[11] - https://www.sciencedirect.com/science/article/abs/pii/S0747563220301849
[12] - https://www.nature.com/articles/s41598-024-55797-w
[13] - https://pmc.ncbi.nlm.nih.gov/articles/PMC6116942/
[14] - https://news.stanford.edu/stories/2018/10/virtual-reality-can-help-make-people-empathetic
[15] - https://pmc.ncbi.nlm.nih.gov/articles/PMC11795159/
[16] - https://med.stanford.edu/news/insights/2024/04/depression-virtual-reality-vr-headset.html
[17] - https://pmc.ncbi.nlm.nih.gov/articles/PMC8319785/
[18] - https://www.ukforum.cz/en/main-categories/unilife/9842-ondrej-moravec-in-vr-you-engage-in-stories-with-your-own-body
[19] - https://voicesofvr.com/1127-darkening-a-spatial-memoir-on-depression-with-voice-interactions-social-dynamics/
[20] - https://www.labiennale.org/en/cinema/2022/venice-immersive/tmání-darkening
[21] - https://dokweb.net/articles/detail/1383/ondrej-moravec-s-darkening-at-venice-iff
[22] - https://www.darkeningvr.com/about
[23] - https://www.mohw.go.kr/board.es?mid=a20401000000&bid=0032&list_no=1488746&act=view
[24] - https://seoul.czechcentres.cz/en/program/darkening
[25] - https://pmc.ncbi.nlm.nih.gov/articles/PMC11928558/
[26] - https://www.frontiersin.org/journals/psychology/articles/10.3389/fpsyg.2015.01409/full
[27] - https://www.psychiatryadvisor.com/home/topics/mood-disorders/for-depressed-patients-time-seems-slower/
[28] - https://www.sciencedirect.com/science/article/abs/pii/S0165178109002224
[29] - https://pmc.ncbi.nlm.nih.gov/articles/PMC5826190/
[30] - https://www.vice.com/en/article/depression-makes-time-feel-slower/
[31] - https://www.technologynetworks.com/neuroscience/news/meta-study-shows-experience-time-altered-depression-283040
[32] - https://pmc.ncbi.nlm.nih.gov/articles/PMC10503922/
[33] - https://pmc.ncbi.nlm.nih.gov/articles/PMC11248432/
[34] - https://positivepsychology.com/inner-critic-worksheets/
[35] - https://www.mayoclinic.org/diseases-conditions/depression/in-depth/treatment-resistant-depression/art-20044324
[36] - https://www.hopkinsmedicine.org/health/wellness-and-prevention/natural-relief-for-depression
[37] - https://pmc.ncbi.nlm.nih.gov/articles/PMC9389105/
[38] - https://pmc.ncbi.nlm.nih.gov/articles/PMC12175210/
[39] - https://www.sciencedirect.com/science/article/pii/S0897189724000387
[40] - https://www.pbs.org/video/vr-training-social-workers-4ijyzx/
[41] - https://socialwork.uky.edu/uk-social-work-launches-virtual-reality-child-welfare-investigation-simulation/
[42] - https://miamioh.edu/news/2025/11/immersive-vr-tech-transforms-how-miami-trains-the-next-generation-of-social-workers.html
[43] - https://www.apa.org/topics/psychotherapy/virtual-reality-group-therapy
[44] - https://www.xr.health/us/blog/virtual-reality-support-groups-anonymous-group-therapy-from-the-comfort-of-home/
[45] - https://www.brainsway.com/knowledge-center/virtual-reality-and-depression/
[46] - https://pmc.ncbi.nlm.nih.gov/articles/PMC9380172/
[47] - https://pmc.ncbi.nlm.nih.gov/articles/PMC11958971/
[48] - https://www.sheehan.com/news/health-in-a-headset-virtual-reality-therapy-and-how-to-avoid-its-legal-and-practical-pitfalls/
[49] - https://pmc.ncbi.nlm.nih.gov/articles/PMC7232669/
[50] - https://pmc.ncbi.nlm.nih.gov/articles/PMC12561320/
[51] - https://pmc.ncbi.nlm.nih.gov/articles/PMC11536554/
[52] - https://pmc.ncbi.nlm.nih.gov/articles/PMC9116500/
[53] - https://pmc.ncbi.nlm.nih.gov/articles/PMC11231641/
[54] - https://www.nationalelfservice.net/treatment/digital-health/immersive-virtual-reality-for-the-treatment-of-mental-health-disorders/
[55] - https://pmc.ncbi.nlm.nih.gov/articles/PMC7366939/
[56] - https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0320215
[57] - https://pmc.ncbi.nlm.nih.gov/articles/PMC11409613/
[58] - https://www.psychedtopractice.com/blog/emerging-applications-and-benefits-of-virtual-reality-in-therapy
If you’re ready to spend less time on documentation and more on therapy, get started with a free trial today
Not medical advice. For informational use only.
Outline
More articles